- There are two main groups of diffuse breast cancers:
- That present as large areas of architectural distortion on the mammogram:
- Neoductgenesis
- Diffusely infiltrating carcinoma:
- Which makes up approximately 5% of all breast cancers
- That present as large areas of architectural distortion on the mammogram:
- When the tumor is e-cadherin negative:
- It is usually called invasive “lobular” carcinoma
- When it is e-cadherin positive:
- It is called infiltrating “ductal” carcinoma
- The designation based on e-cadherin staining is arbitrary:
- Because the behavior of diffusely invasive carcinoma:
- Is the same regardless of the staining
- Because the behavior of diffusely invasive carcinoma:
- Lacking calcifications and a central tumor mass:
- These cancers are notoriously difficult to perceive on mammogram:
- Even when they are large and palpable or when they occur in fatty involuted breasts:
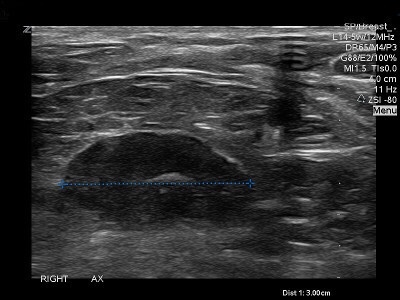
- However, the associated connective tissue response:
- Makes this type of cancer quite visible with ultrasound
- However, the associated connective tissue response:
- Even when they are large and palpable or when they occur in fatty involuted breasts:
- These cancers are notoriously difficult to perceive on mammogram:
- In contrast to diffusely infiltrating cancers:
- Circular (Image 1) and spiculated (Image 2):
- Tumors arising in the terminal ductal lobular units (TDLU) have:
- Bulging, convex contours protruding into the adipose tissue
- Tumors arising in the terminal ductal lobular units (TDLU) have:
- Circular (Image 1) and spiculated (Image 2):
- The solid variety of infiltrating lobular carcinoma:
- Most probably arises within the TDLU:
- Has a circular / oval shape on breast imaging (Images 3)
- Most probably arises within the TDLU:
Image 1: Lobulated spherical tumor mass
Image 2: Multifocal stellate invasive breast cancer
Image 3: Mammographic, MRI and pathologic images of the solid form of invasive lobular
- There are two other variants of invasive lobular carcinoma that arise in the TDLUs:
- The tubulolobular variant:
- Is either a unifocal or multifocal spiculated lesion on the mammogram (Image 5)
- The tubulolobular variant:
Image 4: Mammogram and large format histology of a multifocal tubulolobular breast
- The alveolar type of invasive lobular carcinoma:
- Is usually mammographically occult;
- Or it can be seen as a subtle, asymmetric density (Image 5)
- Is usually mammographically occult;
Image 5: Mammogram and large format histology alveolar type invasive lobular carcinoma
- The various forms of invasive lobular carcinoma that develop in the TDLUs and present as localized lesions:
- Have a significantly better prognosis than the diffusely infiltrating type breast cancer
- Complex sclerosing lesions:
- Present mammographically as non-palpable architectural distortion with no central tumor mass and lucent radiating structures, the so called “black star”:
- As opposed to cancers originating from the TDLU:
- Which have a dense central tumor mass surrounded by radiopaque spiculation, giving the impression of looking at a “white star
- As opposed to cancers originating from the TDLU:
- Present mammographically as non-palpable architectural distortion with no central tumor mass and lucent radiating structures, the so called “black star”:
- Malignant phyllodes tumors:
- Present as large, high density masses:
- The borders may be circumscribed or ill defined
- Present as large, high density masses:
- Fat necrosis:
- Also presents as a hypoechoic, high-density mass
- References
- Tot T. Diffuse invasive breast carcinoma of no special type. Virchows Arch. 2016;468(2):199-206.
- Tabár L, Dean PB. Teaching Atlas of Mammography. New York, NY: Thieme; 2011.
- sity mass.