Blog
Art Show Miami Florida

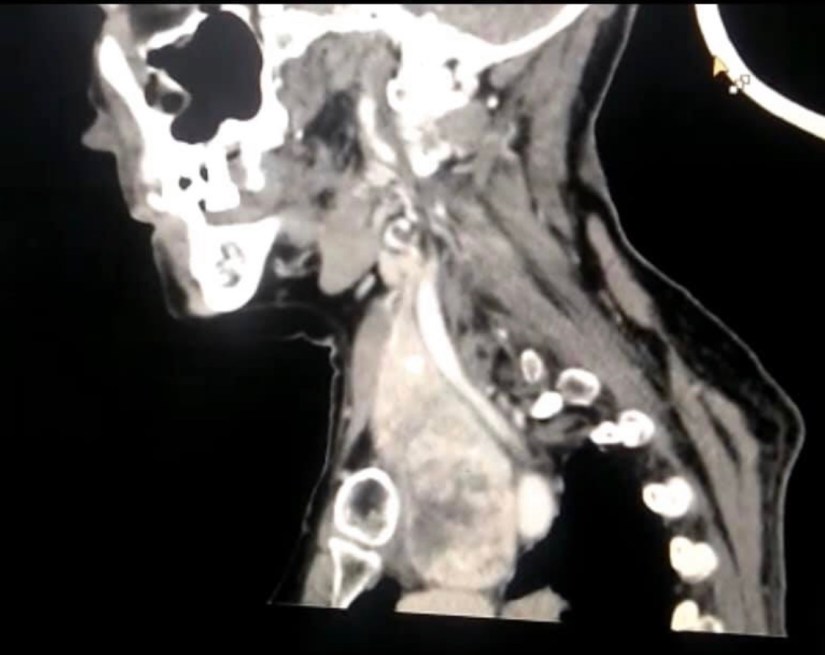
CT Scanning is Indicated for Retrosternal Goiter
- CT scanning is indicated for retrosternal goiter and can provideinformation on the following:
- Confirmation of the presence and determination of extent of retrosternal extension
- A ‘road map’ for the anesthetist:
- Tracheal deviation and compression
- Esophageal compression
- At-risk anatomical structures in the impending surgical field
- An assessment of malignancy (not accessible by ultrasound)
- Anterior versus posterior mediastinal extension
- The likelihood that the goiter can be extracted without the need for a sternotomy:
- The ‘shape’ of the goiter
#Arrangoiz #ThyroidSurgeon #ThyroidExpert #Goiter #ThyroidSurgery #CancerSurgeon #HeadandNeckSurgeon #SurgicalOncologist #Teacher #Surgeon #Miami #Mexico #MountSinaiMedicalCenter
Indications for treatment of goiter include the following:
– Suspicion of malignancy
– Compression of the trachea
– Compression of the esophagus
– Quality of life
#Arrangoiz #ThyroidSurgeon #ThyroidExpert #HeadandNeckSurgeon #MultinodularGoiter #Goiter #Miami #MountSinaiMedicalCenter #Mexico
Prevalence, Pathogenesis, and Natural History of Multinodular / Substernal Goiter
- Multinodular goiter affects:
- 4% of the U.S. population and up to 10% of the British population
- New thyroid nodular disease occurs in:
- 0.1% to 1.5% of the general population per year
- Globally, iodine deficiency contributes to the majority of cases of multinodular goiter:
- It is estimated to affect 1.5 billion people:
- Or nearly 30% of the world’s population in 1990
- It is estimated to affect 1.5 billion people:
- Further, it is estimated that approximately:
- 655 million people in 118 countries are affected by endemic goiter:
- Endemic goiter regions are defined as:
- Iodine-deficient regions in which at least 5% to 10% of the population is affected by goiter
- In certain iodine-deficient regions, higher goiter rates occur:
- In 1994, in Bangladesh, approximately 47% of the population was affected by endemic goiter
- Endemic goiter regions are defined as:
- The majority of the natural iodine supply exists as iodide in the world’s oceans:
- It is therefore mainly non-coastal mountainous and lowland regions:
- Where iodine is leached from the soil by flooding, heavy rainfall, and deforestation that are at risk for endemic goiter
- It is therefore mainly non-coastal mountainous and lowland regions:
- 655 million people in 118 countries are affected by endemic goiter:
- Sporadic forms of multinodular goiter do occur in iodine-replete regions with lesser prevalence:
- Prevalence estimates of sporadic goiters vary between authors:
- Ranging from less than 4% (clinical evaluation series) and between 16% and 67% (ultrasound series)
- Prevalence estimates of sporadic goiters vary between authors:
- Based on tuberculosis screening radiography in Australia and in the United States, substernal goiter has been estimated:
- To be present in 0.02% of general population and 0.05% of females older than 40
- The incidence of substernal goiter was found to significantly increase with age:
- With 60% of substernal goiters occurring in patients older than age 60
- Rates of substernal goiter in the past several decades appear to be decreasing, perhaps related to:
- The introduction of iodized salt, thyroid hormone suppressive therapy, radioiodine use in selective cases, and perhaps more sensitive detection and earlier intervention
- Substernal goiter, as a percentage of patients undergoing thyroidectomy, ranges depending on the series:
- From less than 1% to greater than 20%, with most suggesting a rate of approximately 10%
- Substernal goiters represent approximately:
- 5% of all mediastinal tumors
- Pathogenesis
- The pathogenesis of goiter formation has classically relied on the notion that iodine deficiency promotes persistent elevated thyroid-stimulating hormone (TSH) levels:
- Inducing diffuse thyroid enlargement through thyrocyte proliferation
- Nodules form in the enlarged thyroid as the patient ages, eventually giving rise to multinodular goiter
- Since the early 2000s, this classic model has been challenged by the view that the thyroid gland has an intrinsic propensity to form nodules over time:
- In this new model, low iodine levels and elevated TSH are considered additional factors, exacerbating the innate process of nodule formation
- The shift in conceptualization of goiter pathogenesis has stemmed from new cellular models, first proposed by Studer and Derwahl:
- These authors have argued that the development of multinodular goiter, at least in the later stages, is independent of TSH levels
- Nodules arise because thyroid follicles are embryologically derived from polyclonal progenitors and have thus a heterogeneous sensitivity to TSH signaling
- Thyroid follicles have similarly a differential growth response to continuous exposure to goitrogens:
- Explaining the multinodular pattern of goiters
- In addition, thyrocytes may undergo somatic mutations and acquire a distinct growth capacity:
- The contribution of somatic mutations in multinodular goitrogenesis remains, however, controversial
- This is in contrast with rare growth-promoting germline mutations of the TSH receptor gene:
- Which are believed to be pivotal in congenital diffuse goiter with hyperthyroidism
- Importantly, activating mutations in the TSH receptor gene have not been associated with an increased risk of malignancy
- The pathogenesis of goiter formation has classically relied on the notion that iodine deficiency promotes persistent elevated thyroid-stimulating hormone (TSH) levels:
- Natural History
- The natural history of untreated, sporadic, nontoxic goiter is not completely understood:
- But slow growth appears to be the general predictable pattern:
- Berghout et al. suggested a steady volume increase of up to 10% to 20% per year
- But slow growth appears to be the general predictable pattern:
- Pregnancy, iodine deficiency, consumption of goitrogens, and alteration in suppressive or anti-thyroid medical regimens can result in goiter progression
- Hemorrhage into a preexisting nodule:
- Can also result in the development of acute, regional, and airway symptoms
- In patients presenting with diffuse goiter:
- There is a general tendency toward nodule formation and progressive autonomy:
- With hyperthyroidism ultimately developing in up to 10% of patients
- There is a general tendency toward nodule formation and progressive autonomy:
- The natural history of untreated, sporadic, nontoxic goiter is not completely understood:
- Most substernal goiters arise in the setting of preexisting cervical goiter:
- It is of note, however, that some patients with substernal goiter have no significant cervical goiter component
- Substernal goiters virtually always have a connection to the cervical orthotopic gland
- Lahey, in his experience of approximately 24,000 goiter surgeries, believed that all substernal goiters arise from the cervical gland and maintain their cervical blood supply:
- Even in cases of extreme substernal goiter extending to the diaphragm, the mediastinal component has been found to contain connections to the cervical gland and a blood supply from the inferior thyroid artery
- Connection to the cervical gland may be robust or attenuated, but it virtually always exists
- The work of Torre, based on an impressive series of 237 substernal goiters:
- Suggests that substernal goiters arise 10 years after cervical goiter presentation:
- Suggesting that substernal goiter evolves from preexisting cervical goiter in most cases
- Suggests that substernal goiters arise 10 years after cervical goiter presentation:
- The inferior extension of cervical goiter and formation of substernal goiters is poorly understood:
- The inferior descent relates in part to the pattern of nodular disease within the cervical gland
- Inferior progression results from a limitation of the strap muscles anteriorly, trachea medially, and vertebral column posteriorly:
- As Lahey and Swinton have described, the neck is “a space with no bottom”
- The repetitive forces of deglutition, respiratory dynamics, negative intrathoracic pressure, and gravitational forces in the setting of permissive mediastinal and neck base fascial planes:
- Facilitate the downward extension of cervical goiter
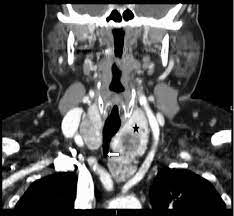
- Typically, anterior mediastinal extension (substernal goiter type I):
- Occurs from the ipsilateral lobe’s inferior expansion
- Descent associated with significant retrotracheal posterior mediastinal extension may arise from more posterior elements of the thyroid gland such as posterior tubercles of Zuckerkandel
#Arrangoiz #ThyroidSurgeon #ThyroidExpert #MultinodularGoiter #Goiter #SubsternalGoiter #HeadandNeckSurgeon #MountSinaiMedicalCenter #Miami #Mexico
Goiter
WHAT ARE THE SYMPTOMS OF A GOITER?
The term “goiter” simply refers to the abnormal enlargement of the thyroid gland. It is important to know that the presence of a goiter does not necessarily mean that the thyroid gland is malfunctioning. A goiter can occur in a gland that is producing too much hormone (hyperthyroidism), too little hormone (hypothyroidism), or the correct amount of hormone (euthyroidism). A goiter indicates there is a condition present which is causing the thyroid to grow abnormally
One of the most common causes of goiter formation worldwide is iodine deficiency. While this was a very frequent cause of goiter in the United States many years ago, it is no longer commonly observed. The primary activity of the thyroid gland is to concentrate iodine from the blood to make thyroid hormone. The gland cannot make enough thyroid hormone if it does not have enough iodine. Therefore, with iodine deficiency the individual will become hypothyroid. Consequently, the pituitary gland in the brain senses the thyroid hormone level is too low and sends a signal to the thyroid. This signal is called thyroid stimulating hormone (TSH). As the name implies, this hormone stimulates the thyroid to produce thyroid hormone and to grow in size. This abnormal growth in size produces what is termed a “goiter.” Thus, iodine deficiency is one cause of goiter development. Wherever iodine deficiency is common, goiter will be common. It remains a common cause of goiters in other parts of the world.
Hashimoto’s thyroiditis is a more common cause of goiter formation in the US. This is an autoimmune condition in which there is destruction of the thyroid gland by one’s own immune system. As the gland becomes more damaged, it is less able to make adequate supplies of thyroid hormone. The pituitary gland senses a low thyroid hormone level and secretes more TSH to stimulate the thyroid. This stimulation causes the thyroid to grow, which may produce a goiter.
Another common cause of goiter is Graves’ disease. In this case, one’s immune system produces a protein, called thyroid stimulating immunoglobulin (TSI). As with TSH, TSI stimulates the thyroid gland to enlarge producing a goiter. However, TSI also stimulates the thyroid to make too much thyroid hormone (causes hyperthyroidism). Since the pituitary senses too much thyroid hormone, it stops secreting TSH. In spite of this the thyroid gland continues to grow and make thyroid hormone. Therefore, Graves’ disease produces a goiter and hyperthyroidism.
Multinodular goiters are another common cause of goiters. Individuals with this disorder have one or more nodules within the gland which cause thyroid enlargement. This is often detected as a nodular feeling gland on physical exam. Patients can present with a single large nodule or with multiple smaller nodules in the gland when first detected. Thus, in early stages of a multinodular goiter with many small nodules, the overall size of the thyroid may not be enlarged yet. Unlike the other goiters discussed, the cause of this type of goiter is not well understood.
In addition to the common causes of goiter, there are many other less common causes. Some of these are due to genetic defects, others are related to injury or infections in the thyroid, and some are due to tumors (both cancerous and benign tumors).
As mentioned earlier, the diagnosis of a goiter is usually made at the time of a physical examination when an enlargement of the thyroid is found. However, the presence of a goiter indicates there is an abnormality of the thyroid gland. Therefore, it is important to determine the cause of the goiter. As a first step, you will likely have thyroid function tests to determine if your thyroid is underactive or overactive. Any subsequent tests performed will be dependent upon the results of the thyroid function tests. If the thyroid is diffusely enlarged and you are hyperthyroid, your doctor will likely proceed with tests to help diagnose Graves’ Disease.
If you are hypothyroid, you may have Hashimoto’s Thyroiditis and you may get additional blood tests to confirm this diagnosis. Other tests used to help diagnose the cause of the goiter may include a radioactive iodine scan, thyroid ultrasound, or a fine needle aspiration biopsy.
The treatment will depend upon the cause of the goiter. If the goiter was due to a deficiency of iodine in the diet (not common in the United States), you will be given iodine supplementation given in preparations to take by mouth. This will lead to a reduction in the size of the goiter, but often the goiter will not completely resolve.
If the goiter is due to Hashimoto’s Thyroiditis, and you are hypothyroid, you will be given thyroid hormone supplement as a daily pill. This treatment will restore your thyroid hormone levels to normal, but does not usually make the goiter go completely away. While the goiter may get smaller, sometimes there is too much scar tissue in the gland to allow it to get much smaller. However, thyroid hormone treatment will usually prevent it from getting any larger. Although appropriate in some individuals, surgery is usually not routine treatment of thyroiditis.
If the goiter is due to hyperthyroidism, the treatment will depend upon the cause of the hyperthyroidism. For some causes of hyperthyroidism, the treatment may lead to a disappearance of the goiter. For example, treatment of Graves’ disease with radioactive iodine usually leads to a decrease or disappearance of the goiter.
Many goiters, such as the multinodular goiter, are associated with normal levels of thyroid hormone in the blood. These goiters usually do not require any specific treatment after the appropriate diagnosis is made. If no specific treatment is suggested, you may be warned that you are at risk for becoming hypothyroid or hyperthyroid in the future. However, if there are problems associated with the size of the thyroid per se, such as the goiter getting so large that it constricts the airway, your doctor may suggest that the goiter be treated by surgical removal.
Whatever the cause, it is important to have regular (annual) monitoring when diagnosed with a goiter.

#Arrangoiz #ThyroidSurgeon #ThyroidExpert #HeadandNeckSurgeon #ThyroidCancer #Goiter #MountSinaiMedicalCenter #Miami #Mexico
New Appointment

Rodrigo Arrangoiz MS, MD, FACS, FSSO
Assistant Professor at the Columbia University Division of Surgical Oncology at Mount Sinai Medical Center
Multiple Endocrine Neoplasia Type 1 (Wermer Syndrome)
- The earliest and most common presentation of MEN type 1 (Wermer Syndrome):
- Is primary hyperparathyroidism (PHPT):
- Develops in approximately 80% to 100% of patients:
- By age 40 years
- Develops in approximately 80% to 100% of patients:
- Is primary hyperparathyroidism (PHPT):
- Patients with MEN type 1 also are predisposed to the development of:
- Pancreatic neuroendocrine tumors
- Pituitary adenomas
- Less frequently:
- Skin angiomas
- Lipomas
- Adrenocortical tumors
- Neuroendocrine tumors of the:
- Thymus
- Bronchus
- Stomach
- MEN type 1 has been shown to result from:
- A germline mutation in a tumor suppressor gene:
- Called MEN1 gene:
- Located on chromosome 11q12-13:
- That encodes Menin:
- A protein that is postulated to interact with:
- The transcription factors JunD and nuclear factor-κB in the nucleus
- In addition to replication protein A and other proteins
- A protein that is postulated to interact with:
- That encodes Menin:
- Located on chromosome 11q12-13:
- Called MEN1 gene:
- A germline mutation in a tumor suppressor gene:
- Pre-symptomatic screening for mutation carriers for MEN type 1:
- Is difficult because generally MEN1 mutations result in a:
- Nonfunctional protein:
- That are scattered throughout the translated nine exons of the gene
- Nonfunctional protein:
- Is difficult because generally MEN1 mutations result in a:
- MEN1 mutations also have been found in:
- Kindred’s initially suspected to represent isolated familial HPT
- Screening for mutation carriers for MEN type 1:
- Has a very high detection rate greater than 94%, and is used in Sweden for patients with:
- PHPT with a first-degree relative with a major endocrine tumor, age of onset is less than 30 years and / or if multiple pancreatic tumors / or when parathyroid hyperplasia is detected
- Has a very high detection rate greater than 94%, and is used in Sweden for patients with:
#Arrangoiz #ParathyroidSurgeon #ParathyroidExpert #Hyperparathyroidism #PrimaryHyperparathyroidism #CancerSurgeon #EndocrineSurgery #Teacher #Surgeon #HeadandNeckSurgeon #SurgicalOncologist #ParathyroidAdenoma #Hypercalcemia #ElevatedCalciumLevels #Miami #MountSinaiMedicalCenter #MSMC #Mexico #Hialeah
American Association of Endocrine Surgeons Guidelines for the Management of Hyperparathyroidism in Patients with MEN Type 1 (Wermer Syndrome) and MEN Type IIa (Simple Syndrome)
- Per the American Association of Endocrine Surgeons guidelines:
- The initial operation for hyperparathyroidism in patients with MEN type 1 should be:
- Subtotal parathyroidectomy
- While in MEN type IIa patients:
- Only visibly enlarged glands need to be removed
- The initial operation for hyperparathyroidism in patients with MEN type 1 should be:
- https://jamanetwork.com/journals/jamasurgery/fullarticle/2542667
#Arrangoiz #ParathyroidSurgeon #ParathyroidExpert #Hyperparathyroidism #PrimaryHyperparathyroidism #CancerSurgeon #EndocrineSurgery #Teacher #Surgeon #HeadandNeckSurgeon #SurgicalOncologist #ParathyroidAdenoma #Hypercalcemia #ElevatedCalciumLevels #Miami #MountSinaiMedicalCenter #MSMC #Mexico #Hialeah