👉JAMA Surg. Published online November 6, 2019. doi:10.1001/jamasurg.2019.4613
– Question : Do intraoperative imaging systems using near-infrared autofluorescence light to identify parathyroid glands influence parathyroid preservation and postoperative hypocalcemia?
👉Findings: In this randomized clinical trial of 241 adults, the use of near-infrared autofluorescence during total thyroidectomy helped lower the temporary postoperative hypocalcemia rate from 22% to 9% and the parathyroid autotransplantation and parathyroid inadvertent resection rates from 16% to 4% and 14% to 3%, respectively.
👉Meaning: Near-infrared autofluorescence–based identification of parathyroid glands during thyroid surgery may limit parathyroid risk.
👉Importance Because inadvertent damage of the parathyroid glands can lead to postoperative hypocalcemia, their identification and preservation, which can be challenging, are pivotal during total thyroidectomy.
👉Objective To determine if intraoperative imaging systems using near-infrared autofluorescence (NIRAF) light to identify parathyroid glands could improve parathyroid preservation and reduce postoperative hypocalcemia.
👉Design, Setting, and Participants This randomized clinical trial was conducted from September 2016 to October 2018, with a 6-month follow-up at 3 referral hospitals in France. Adult patients who met eligibility criteria and underwent total thyroidectomy were randomized. The exclusion criteria were preexisting parathyroid diseases.
👉Interventions Use of intraoperative NIRAF imaging system during total thyroidectomy.
👉Main Outcomes and Measures The primary outcome was the rate of postoperative hypocalcemia (a corrected calcium <8.0 mg/dL [to convert to mmol/L, multiply by 0.25] at postoperative day 1 or 2). The main secondary outcomes were the rates of parathyroid gland autotransplantation and inadvertent parathyroid gland resection.
👉Results A total of 245 of 529 eligible patients underwent randomization. Overall, 241 patients were analyzed for the primary outcome (mean [SD] age, 53.6 [13.6] years; 191 women [79.3%]): 121 who underwent NIRAF-assisted thyroidectomy and 120 who underwent conventional thyroidectomy (control group). The temporary postoperative hypocalcemia rate was 9.1% (11 of 121 patients) in the NIRAF group and 21.7% (26 of 120 patients) in the control group (between-group difference, 12.6% [95% CI, 5.0%-20.1%]; P= .007). There was no significant difference in permanent hypocalcemia rates (0% in the NIRAF group and 1.6% [2 of 120 patients] in the control group). Multivariate analyses accounting for center and surgeon heterogeneity and adjusting for confounders, found that use of NIRAF reduced the risk of hypocalcemia with an odds ratio of 0.35 (95% CI, 0.15-0.83; P= .02). Analysis of secondary outcomes showed that fewer patients experienced parathyroid autotransplantation in the NIRAF group than in the control group: respectively, 4 patients (3.3% [95% CI, 0.1%-6.6%) vs 16 patients (13.3% [95% CI, 7.3%-19.4%]; P= .009). The number of inadvertently resected parathyroid glands was significantly lower in the NIRAF group than in the control group: 3 patients (2.5% [95% CI, 0.0%-5.2%]) vs 14 patients (11.7% [95% CI, 5.9%-17.4%], respectively; P= .006).
👉Conclusions and Relevance The use of NIRAF for the identification of the parathyroid glands may help improve the early postoperative hypocalcemia rate significantly and increase parathyroid preservation after total thyroidectomy.
Trial Registration ClinicalTrials.gov identifier: NCT02892253
The use of NIRAF for the identification of the PGs helped improve the early postoperative hypocalcemia rate significantly and increased parathyroid preservation after total thyroidectomy. https://ja.ma/2PS7zdN
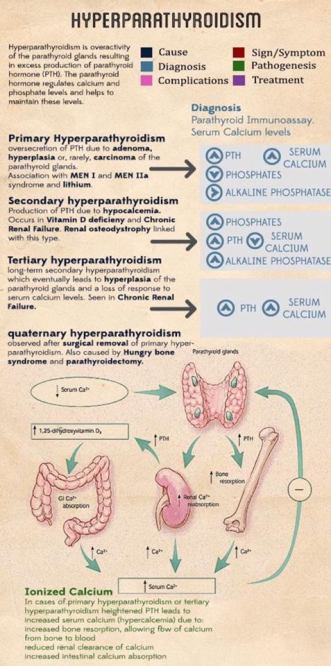
 Rodrigo Arrangoiz MS, MD, FACS cirujano de tumores de cabeza y cuello / cirugia endocrina es experto en el manejo del hiperparatiroidismo primario.
Rodrigo Arrangoiz MS, MD, FACS cirujano de tumores de cabeza y cuello / cirugia endocrina es experto en el manejo del hiperparatiroidismo primario.
 Introdujo a nuestro país la técnica de exploración bilateral de cuello con valoración de la funcionalidad de las glándulas paratiroides con paratiroidectomia radioguiada:
Introdujo a nuestro país la técnica de exploración bilateral de cuello con valoración de la funcionalidad de las glándulas paratiroides con paratiroidectomia radioguiada:
https://m.youtube.com/watch?v=AgvQmtz1gnA&time_continue=127
 Su entrenamiento fue el siguiente:
Su entrenamiento fue el siguiente:
• Cirugia general y gastrointestinal:
• Michigan State University:
• 2004 al 2010 • Cirugia oncológica / tumores de cabeza y cuello / cirugia endocrina:
• Cirugia oncológica / tumores de cabeza y cuello / cirugia endocrina:
• Fox Chase Cancer Center (Filadelfia):
• 2010 al 2012 • Maestria en ciencias (Clinical research for healthprofessionals):
• Maestria en ciencias (Clinical research for healthprofessionals):
• Drexel University (Filadelfia):
• 2010 al 2012 • Cirugia de tumores de cabeza y cuello / cirugiaendocrina
• Cirugia de tumores de cabeza y cuello / cirugiaendocrina
• IFHNOS / Memorial Sloan Kettering Cancer Center:
• 2014 al 2016
http://www.sociedadquirurgica.com
http://www.hiperparatiroidismo.info
#Arrangoiz
#CirugiadeTumoresdeCabezayCuello
#CirugiaEndocrina
#CirugiaOncologica
#HeadandNeckSurgery
#EndocrineSurgery
#SurgicalOncology
#Hyperparathyroidism
#Hiperparatiroidismo