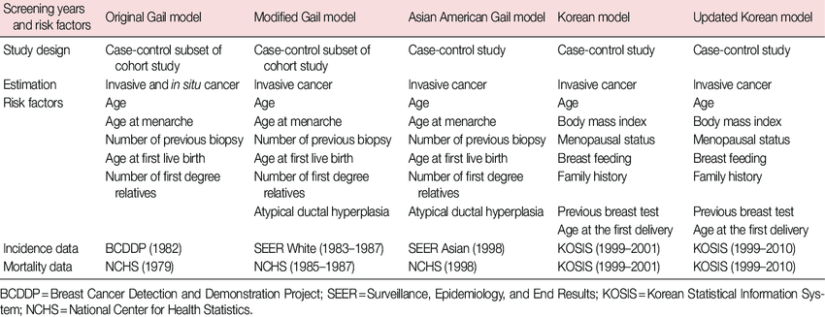
- The Gail Model:
- Is a statistical breast cancer risk assessment algorithm:
- That was developed in 1989 by Dr. Mitchell Gail and colleagues:
- From the Biostatistics Branch of the National Cancer Institute’s Division of Cancer Epidemiology and Genetics
- That was developed in 1989 by Dr. Mitchell Gail and colleagues:
- It was derived from a huge screening study of:
- 280,000 women
- 35 to 74 years of age
- The Gail model has proved to be:
- A reasonable tool for estimating breast cancer risk in white women,
- Other researchers have subsequently supplemented the model to provide accurate risk assessments for African-American, Hispanic, and Asian women.
- However, the Gail model:
- Underestimates the breast cancer risk for women with:
- A significant family history:
- Consequently, it should not be used for women:
- Suspected to have a hereditary syndrome associated with increased risk of breast cancer
- Consequently, it should not be used for women:
- A significant family history:
- Underestimates the breast cancer risk for women with:
- The Gail Model looked at:
- A woman’s personal medical history, familial history, and reproductive history:
- These variables were then adjusted:
- According to age and associated higher risk for older women
- These variables were then adjusted:
- A woman’s personal medical history, familial history, and reproductive history:
- The Gail Model is a risk prediction tool that is designed to:
- Derive individual risk estimates for the development of breast cancer over time
- It was developed to estimate the probability of developing breast cancer over a defined age interval
- It was also intended to improve screening guidelines
- However, the Gail model did not take into account:
- Racial or ethnic differences
- The risk of women with atypical hyperplasia on a breast biopsy (atypia),
- BRCA genetic variants
- Tamoxifen use
- In addition:
- It excluded women who had already had a confirmed diagnosis of either:
- Ductal or lobular breast carcinoma in situ
- It excluded women who had already had a confirmed diagnosis of either:
- In 2008, the accuracy of the Gail Model for women with a history of atypia was reported:
- Women with atypia were identified from the Mayo Benign Breast Disease (BBD) cohort (1967 to 1991)
- Their risk factors for breast cancer were obtained, and the Gail Model was used to predict 5-year– and follow-up–specific risks for each woman. The predicted and observed numbers of breast cancers were compared, and the concordance between individual risk levels and outcomes was computed
- Of the 9,376 women in the BBD cohort:
- 331 women had atypia (3.5%)
- At a mean follow-up of 13.7 years:
- 58 of 331 (17.5%) patients had developed invasive breast cancer, 1.66 times more than the 34.9 predicted by the Gail model (95% confidence index [CI], 1.29 to 2.15; P < 0.001).
- For individual women, the concordance between predicted and observed outcomes was low, with a concordance statistic of 0.50 (95% CI, 0.44 to 0.55):
- The C-statistic (sometimes called the “concordance” statistic or C-index):
- Is a measure of goodness of fit for binary outcomes in a logistic regression model
- In clinical studies, the C-statistic gives the probability a randomly selected patient who experienced an event (eg, a disease or condition) had a higher risk score than a patient who had not experienced the event:
- A concordance statistic of 0.5 means that the predication ability of the Gail Model was no better than chance for women with abnormal biopsy results in the past
- The C-statistic (sometimes called the “concordance” statistic or C-index):
- However, the model was subsequently revised (Gail Model 2) and validated to predict risk of invasive breast cancer:
- Including information on the history of first-degree affected family members
- The Gail Model 2 has been used extensively in clinical practice and has served as the basis for eligibility for a number of the breast cancer prevention trials
- The US Food and Drug Administration (FDA) guidelines:
- Use the National Surgical Adjuvant Breast and Bowel Project’s (NSABP) modified Gail model:
- As the basis for eligibility for the prophylactic use of tamoxifen
- Tamoxifen, a selective estrogen receptor modulator (SERM):
- Is approved for:
- Women aged 35 years and older
- Who have a 5-year modified Gail risk of breast cancer of:
- 1.67% or more
- Is approved for:
- Use the National Surgical Adjuvant Breast and Bowel Project’s (NSABP) modified Gail model:
- The Gail Model 2 also forms the basis of the:;
- The Gail Model 2 is most accurate for:
- Non-Hispanic white women who receive annual mammograms:
- But the model tends to overestimate risk in younger women who do not receive annual mammograms
- The model also demonstrates reduced accuracy in populations with:
- Demographics (ie, age, race, extent of screening) that differ from the population on which it was built
- At the individual level:
- The model lacks adequate discrimination in predicting risk and has been challenged on its generalizability across populations
- The updated Gail Model Calculator (which incorporates information for women of other races and ethnicities):
- Also known as the Breast Cancer Risk Assessment Tool:
- Is available online at the National Cancer Institute website:
- Also known as the Breast Cancer Risk Assessment Tool:
- To address concerns regarding applicability of the modified Gail model to black women:
- Gail and colleagues derived a model using data from a large case-control study of black women participating in the Women’s Contraceptive and Reproductive Experiences (CARE) study
- The CARE model demonstrated high concordance between the number of breast cancers predicted and the number of breast cancers observed among black women when validated in the WHI cohort
- The CARE model better estimates the risk in black women (whereas the Gail model underestimates breast cancer risk in them) and can be additive to other factors (such as family history, genomics, and environmental factors) when assessing risk and providing counsel for black women
- Non-Hispanic white women who receive annual mammograms:
- Is a statistical breast cancer risk assessment algorithm:
- Rodrigo Arrangoiz MS, MD, FACS cirujano oncology y cirujano de mamá de Sociedad Quirúrgica S.C en el America British Cowdray Medical Center en la ciudad de Mexico:
- Es experto en el manejo del cáncer de mama.

👉Es miembro de la American Society of Breast Surgeons:

Training:
• General surgery:
• Michigan State University:
• 2004 al 2010
• Surgical Oncology / Head and Neck Surgery / Endocrine Surgery:
• Fox Chase Cancer Center (Filadelfia):
• 2010 al 2012
• Masters in Science (Clinical research for health professionals):
• Drexel University (Filadelfia):
• 2010 al 2012
• Surgical Oncology / Head and Neck Surgery / Endocrine Surgery:
• IFHNOS / Memorial Sloan Kettering Cancer Center:
• 2014 al 2016