Classification
👉Multiple endocrine neoplasia type 2 (MEN2) is subclassified into two distinct syndromes: types 2A (MEN2A) and 2B (MEN2B).
👉Within MEN2A, there are four variants:
● Classical MEN2A
● MEN2A with cutaneous lichen amyloidosis (CLA)
● MEN2A with Hirschsprung disease (HD)
● Familial medullary thyroid cancer (FMTC)
👉In both MEN2A and MEN2B, there is an occurrence of multicentric tumor formation in all organs where the RET proto-oncogene is expressed.
👉The thyroid, parathyroid, adrenal glands, and accessory adrenals are at risk for developing tumors that may reduce life expectancy and quality of life.
Multiple endocrine neoplasia type 2A
Classical MEN2A
👉Classical multiple endocrine neoplasia 2A (MEN2A) is the most common MEN2A variant.
👉It is a heritable predisposition to medullary thyroid cancer (MTC), pheochromocytoma, and primary parathyroid hyperplasia.
👉The respective frequency of these tumors in classical MEN2A is over 90% for MTC, approximately 10% to 50% for pheochromocytoma, and 10% to 20% for multigland parathyroid hyperplasia.
👉The frequency of the development of MTC, pheochromocytoma, and parathyroid hyperplasia depends upon the specific RET mutation.
MEN2A with cutaneous lichen amyloidosis
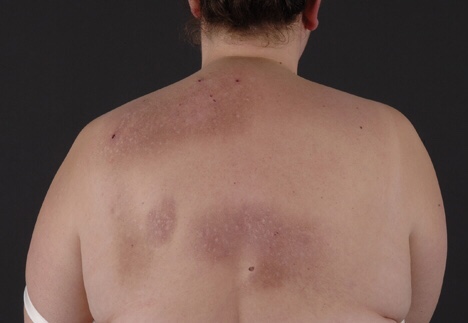
👉CLA (also known as lichen planus amyloidosis [LPA]) has been described in some families with multiple endocrine neoplasia 2A (MEN2A), predominantly those with the RET codon 634 mutation, although it has also been reported in a patient with a codon 804 mutation.
👉The diagnosis of CLA may precede the onset of clinically evident MTC (Image).
👉Patients with this variant develop pheochromocytomas and parathyroid hyperplasia with a similar frequency as those with classical MEN2A.
MEN2A with Hirschsprung disease (HD)
👉HD is a motor disorder of the gut that is caused by the failure of neural crest cells (precursors of enteric ganglion cells) to migrate completely during intestinal development.
👉The resulting aganglionic segment of the colon fails to relax, causing a functional obstruction.
👉At least eight genetic mutations have been identified in patients with HD.
👉The predominant gene affected is the RET proto-oncogene.
👉RET malfunction accounts for at least 50% of familial and 20% of sporadic cases of HD.
👉In one study, the prevalence of HD in MEN2 was 7.5%.
👉The frequency of HD in MEN2A depends upon the specific RET mutation.
👉The co-occurrence of HD and MEN2A is predominantly associated with RET mutations involving codons 609, 611, 618, and 620.
👉In such patients, HD may be the first presentation of MEN2A.
👉Patients with this variant of MEN2A develop MTC, pheochromocytomas, and parathyroid hyperplasia with a similar frequency as those with classical MEN2A.
Familial medullary thyroid cancer
👉FMTC is a variant of MEN2A in which there is a strong predisposition to MTC but not the other clinical manifestations of MEN2A (or 2B).
👉The clinical distinction of FMTC from MEN2A may be difficult on statistical grounds in small families; even in some large kindreds, the clinical designation of FMTC has been changed to MEN2A after the diagnosis of pheochromocytoma or hyperparathyroidism in a family member.
👉Because FMTC is the most limited variant of MEN2, making the wrong diagnosis of FMTC could result in missing a pheochromocytoma in a patient with MEN2.
👉Therefore, an FMTC kindred should be defined using the following rigorous criteria:
● More than 10 carriers in the kindred
● Multiple carriers or affected members over the age of 50 years
● An adequate medical history, particularly in older family members
👉Why pheochromocytomas and hyperparathyroidism infrequently develop in these families is still unknown since many FMTC and MEN2A families carry identical RET mutations.
👉In rare families, both HD and FMTC appear to segregate.
👉In a report summarizing data from 250 Italian kindreds with hereditary MTC, the prevalence of the FMTC phenotype among RET mutation carriers was higher than MEN2A and MEN2B (57%, 34% and 6.8%, respectively).
👉This may be related to the introduction of RET screening in the work-up of apparently sporadic MTC and the more extensive search for RET mutations in non-hot spot regions of the gene.
Multiple endocrine neoplasia type 2B
👉The frequency of MEN2B has been estimated at roughly 6% of all MEN2 patients.
👉MEN2B shares the inherited predisposition to MTC and pheochromocytoma that occurs in MEN2A.
👉On the other hand, parathyroid hyperplasia is not a feature of this disorder.
👉There are additional important clinical differences.
👉Patients with MEN2B tend to have mucosal neuromas, typically involving the lips and tongue, and intestinal ganglioneuromas.
👉Disturbances of colonic function are common, including chronic constipation and megacolon.
👉Many of these patients have development abnormalities, a Marfanoid habitus, and myelinated corneal nerves.
👉MTC is the most common component of the MEN2B syndrome.
👉Furthermore, the tumor is often more aggressive and of earlier onset than in MEN2A; as a result, early diagnosis and prevention are particularly critical.

- What is Head and Neck Surgery?:
- It is a surgical sub-specialty that deals mainly with benign and malignant tumors of the head and neck region, including:
- The scalp, facial region, eyes, ears, nose, nasal fossae, paranasal sinuses, oral cavity, pharynx (nasopharynx, oropharynx, hypopharynx), larynx (supraglotic larynx, glottis larynx, subglotic larynx), thyroid gland, parathyroid gland, salivary glands (parotid glands, submandibular glands, sublingual glands, minor salivary glands), soft tissues of the neck, skin of the head and neck region.
- The head and neck surgeon’s work area:
- Does not cover tumors or diseases of the brain and other areas of the central nervous system or those of the cervical spine:
- This is the neurosurgeon field.
- Does not cover tumors or diseases of the brain and other areas of the central nervous system or those of the cervical spine:
- The head and neck surgeon’s work area:
- The scalp, facial region, eyes, ears, nose, nasal fossae, paranasal sinuses, oral cavity, pharynx (nasopharynx, oropharynx, hypopharynx), larynx (supraglotic larynx, glottis larynx, subglotic larynx), thyroid gland, parathyroid gland, salivary glands (parotid glands, submandibular glands, sublingual glands, minor salivary glands), soft tissues of the neck, skin of the head and neck region.
- Among the diagnostic procedures performed by the head and neck surgeon, are the following:
- Nasopharyngolaryngoscopy:
- Performed to examine, evaluate and, possibly perform a biopsy, of oral cavity, pharyngeal and laryngeal lesions.
- Nasopharyngolaryngoscopy:
- The surgeries most commonly performed by the head and neck surgeon are:
- Total or near total thyroidectomies
- Hemithryoidectomies (lobectomies)
- Comprehensive neck dissections
- Selective neck dissections
- Maxillectomies:
- Total maxillectomy
- Subtotal maxillectomy
- Infrastructure maxillectomy
- Suprastructure maxillectomy
- Medial maxillectomy
- Mandibulectomy:
- Segmental
- Marginal
- Tracheostomy
- Salivary gland surgeries:
- Parotid gland operations:
- Limited superficial parotidectomy with identification and preservation of the facial nerve
- Superficial parotidectomy with identification and preservation of the facial nerve
- Near total parotidectomy with identification and preservation of the facial nerve
- Total parotidectomy
- Submandibular gland resection
- Sublingual gland resection
- Parotid gland operations:
- Resection of tumors of the oral cavity:
- Glossectomy
- Resection of the floor of the mouth tumors
- Resection of tumors of the pharynx
- Resection of tumors of the larynx
- Split-thickness skin grafts
- Full-thickness skin grafts
- Sentinel lymph node mapping and sentinel lymph node biopsy
- Resection of malignant skin tumors (BCC, SCC, melanoma) of the head and neck region
- It is a surgical sub-specialty that deals mainly with benign and malignant tumors of the head and neck region, including:
- The formation of the head and neck surgeon includes mastering the following subjects:
- Surgical Anatomy
- History and Basic Principles of Head and Neck Surgery
- Epidemiology, Etiology, and Pathology of Head and Neck Diseases
- Diagnostic Radiology of the Head and Neck Region
- Tumors of the Scalp, Skin and Melanoma
- Eyelids and Orbit
- Nasal Cavity and Paranasal Sinuses
- Skull Base and Temporal Bone
- Lips and Oral Cavity
- Pharynx and Esophagus
- Larynx and Trachea
- Cervical Lymph Nodes
- Thyroid and Parathyroid Glands
- Salivary Glands
- Neurogenic Tumors and Paragangliomas
- Soft Tissue Tumors
- Bone Tumors and Odontogenic Lesions
- Reconstructive Surgery
- Oncologic Dentistry and Maxillofacial Prosthetics
- Principles of Radiation Oncology
- Principles of Chemotherapy
- Molecular Oncology, Genomics and Immunology
- Nutrition
- Biostatistic
-
Rodrigo Arrangoiz MS, MD, FACS a head and neck surgeon / endocrine surgeon / surgical oncologist and is a member of Sociedad Quirúrgica S.C at the America British Cowdray Medical Center in Mexico City:

- Rodrigo Arrangoiz MS, MD, FACS:
- Is a member of the American Head and Neck Society

-
- He is a member of the American Thyroid Association:





