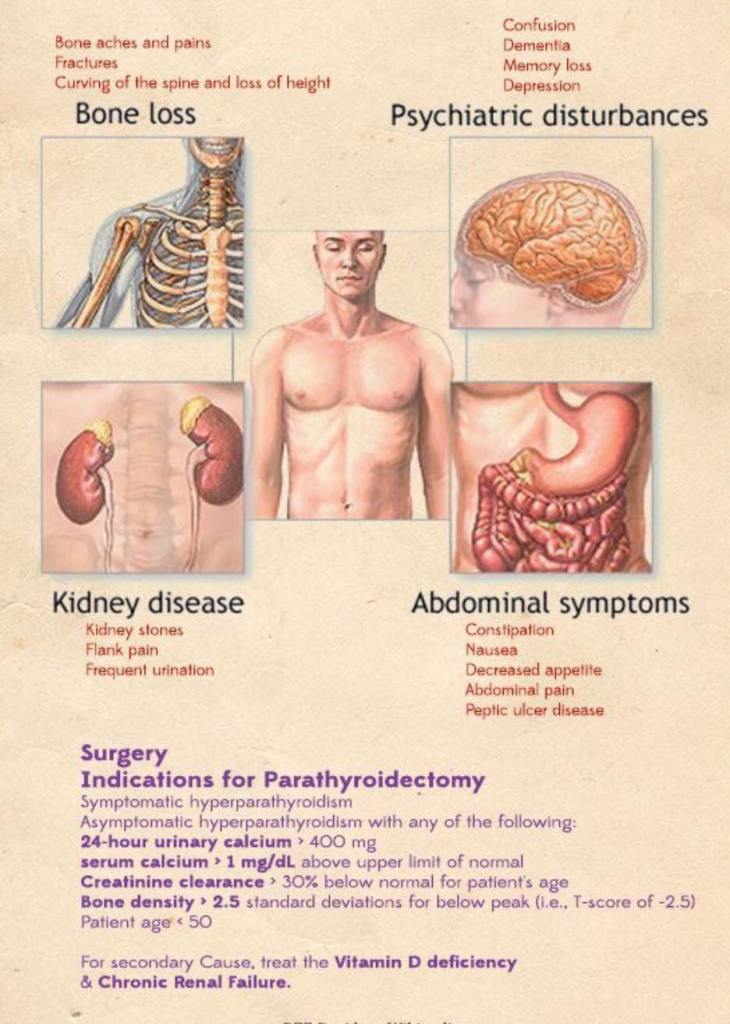
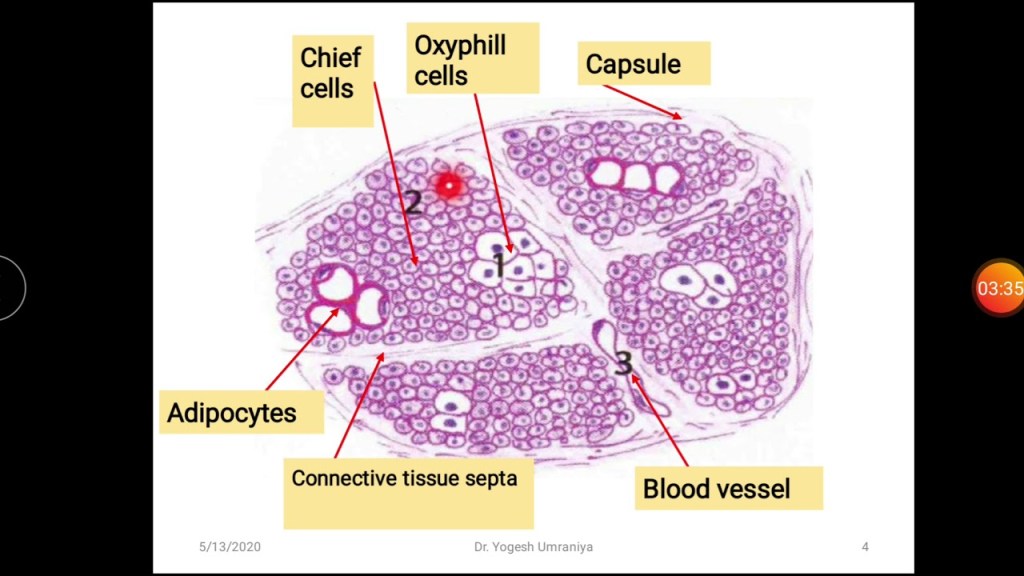
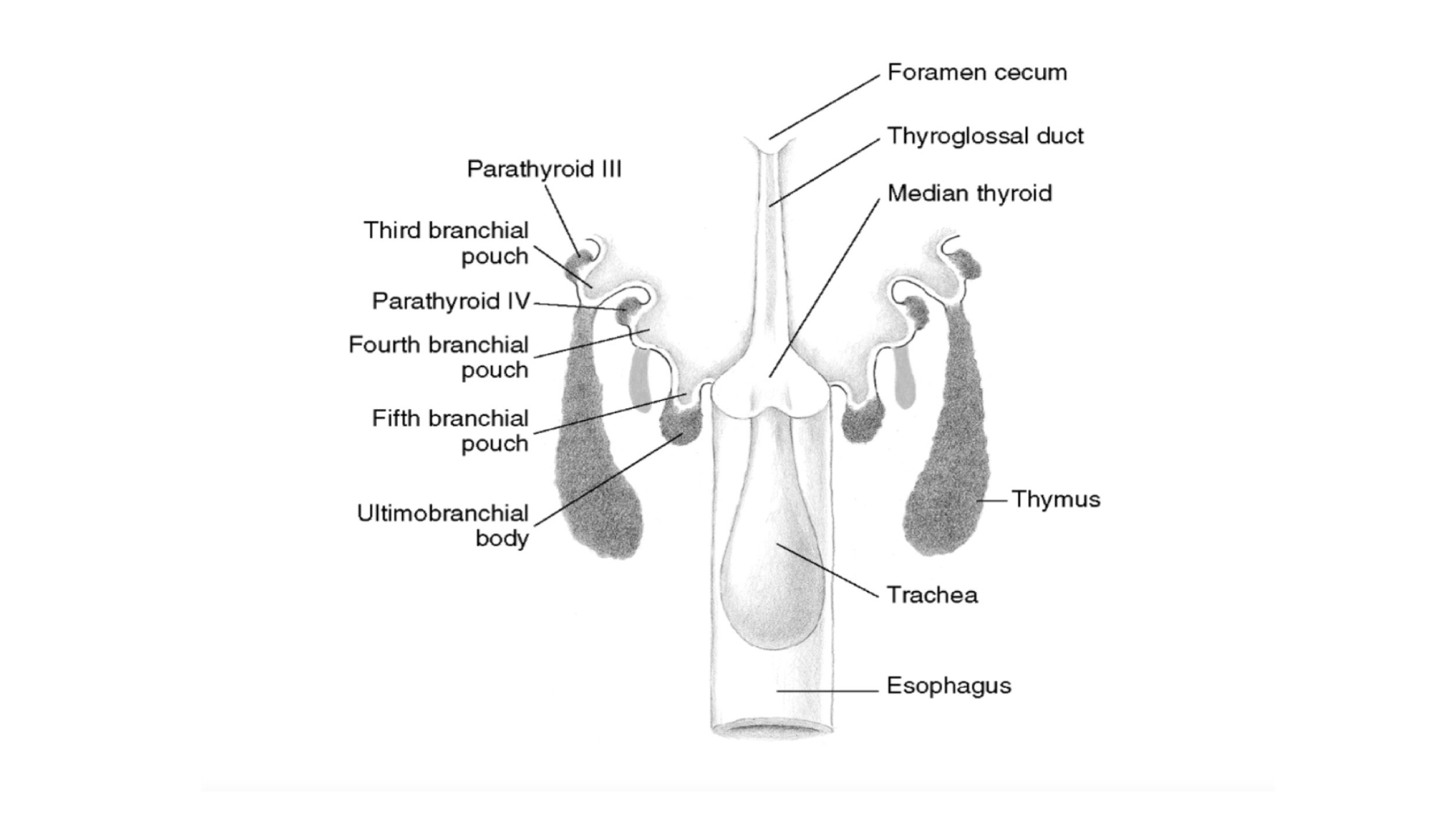
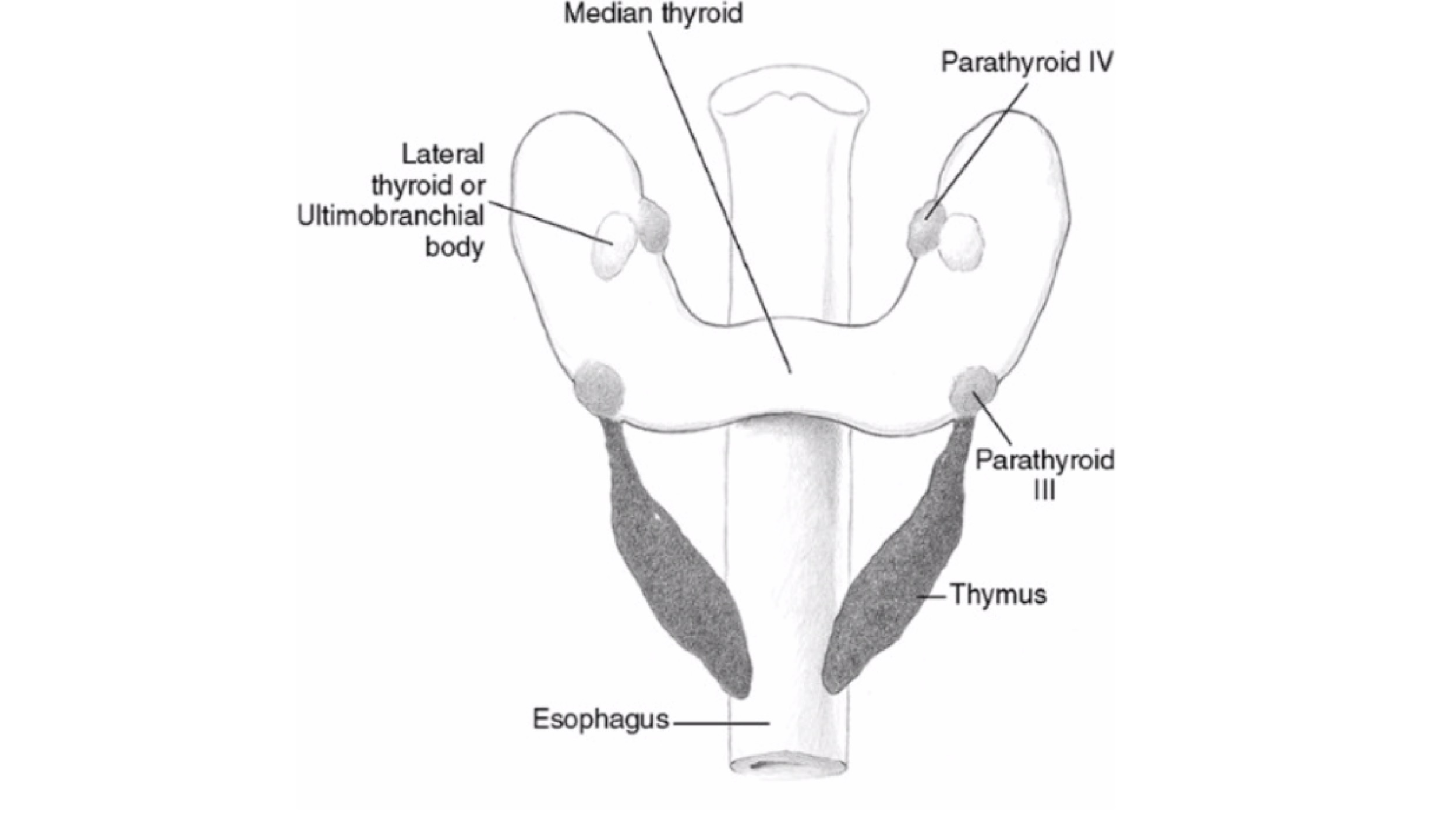
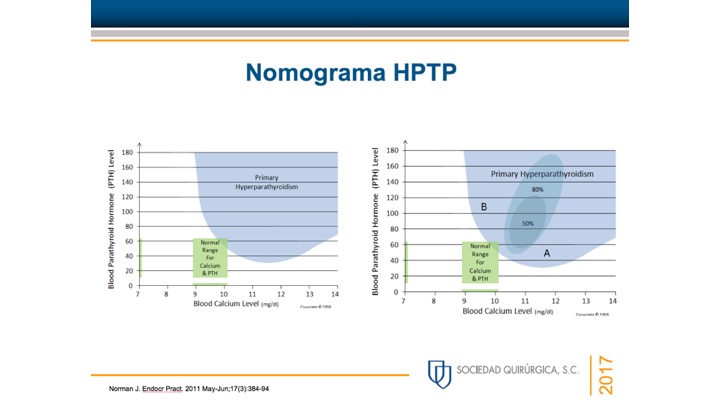
- PHPT is defined as hypercalcemia or widely fluctuating levels of serum calcium levels:
- Resulting from the inappropriate or autogenous secretion of PTH by one or more parathyroid glands:
- In the absence of a known or recognized stimulus
- Resulting from the inappropriate or autogenous secretion of PTH by one or more parathyroid glands:
- The most common cause of hypercalcemia in the outpatient setting is PHPT:
- With approximately 100,000 new cases per year reported in the United States
- Since the advent of routine laboratory testing:
- The prevalence of the disease has increased from 0.1% to 0.4%:
- One to seven cases per 1000 adults
- The prevalence of the disease has increased from 0.1% to 0.4%:
- In a study by Yeh et al., the incidence of PHPT fluctuated between:
- 36.3 and 120.2 cases per 100,000 women-years
- 13.4 and 35.6 in 100,000 men-years
- PHPT may present at any age:
- With the vast majority of cases occurring in patients older than 45 years of years
- Women have consistently made up the preponderance of cases:
- With a female-to-male ratio of:
- 3:1 to 4:1
- Based on a population based study from Rochester Minnesota:
- The higher incidence of this could be secondary (hypothetically) to estrogen deficiency after menopause that reveals underlying HPT
- With a female-to-male ratio of:
- The precise origin of PHPT is unknown:
- Although exposure to low-dose therapeutic ionizing radiation and familial predisposition account for some cases:
- Irradiation for acne could have accounted for a 2 to 3-fold increase in the incidence of this disease at some point in time, and a 4-fold increase was noted in survivors of the atomic bomb
- Schneider et al., in their study of 2555 patients followed for 50 years, even low doses of radiation exposure during the teenage years was associated with a slight risk of developing PHPT:
- In this study a dose response was documented in people receiving external-beam radiotherapy for benign diseases before their 16th birthday
- The latency period for the development of PHPT after radiation exposure is longer than that for the development of thyroid tumors:
- With most cases occurring 30 to 40 years after exposure
- Patients who have been radiated have similar clinical manifestations and serum calcium levels when compared to patients without a history of radiation exposure:
- However, the former tend to have higher PTH levels and a higher incidence of concomitant thyroid neoplasms
- Certain medications have been implicated in the development of hypercalcemia:
- Lithium therapy has been known to shift the set point for PTH secretion in parathyroid cells:
- Thereby resulting in elevated PTH levels and mild hypercalcemia
- Lithium stimulates the growth of abnormal parathyroid glands in vitro and also in susceptible patients in vivo
- Unusual metabolic features associated with lithium use include:
- Low urinary calcium excretion
- Normal cyclic AMP excretion
- Lack of calcic nephrolithiasis
- The mechanism probably results from lithium linking with the calcium sensing receptor on the parathyroid glands:
- Resulting in PTH secretion
- Elevated serum calcium levels have been associated with thiazide diuretic:
- The overall annual age- and sex-adjusted (to 2000 U.S. whites) incidence was:
- 7.7 (95% CI, 5.9 to 9.5) per 100,000 individuals
- The average 24-hour plasma calcium concentrations are increased with thiazide diuretic use:
- But the mean 24-hour PTH levels remain unchanged in subjects with normal baseline PTH levels and no evidence of hypercalciuria
- Thiazides diuretics have several metabolic effects that may contribute to increased calcium levels:
- A decrease in urine calcium excretion is the most likely cause:
- But in some cases diuretic use has been associates with a metabolic alkalosis:
- That could increase the total serum calcium levels through a pH-dependent increase in protein-bound calcium
- Although plasma 1,25 (OH) vitamin D levels are unchanged:
- Increased intestinal calcium absorption in response to thiazide diurectic use has been noted and could also contribute to an increase in serum calcium
- But in some cases diuretic use has been associates with a metabolic alkalosis:
- One last possible explanation for the elevated serum calcium levels associated with thiazide diuretic use is hemoconcentration associated with dieresis
- A decrease in urine calcium excretion is the most likely cause:
- The overall annual age- and sex-adjusted (to 2000 U.S. whites) incidence was:
- Lithium therapy has been known to shift the set point for PTH secretion in parathyroid cells:
- Numerous genetic abnormalities have been identified in the development of PHPT, including anomalies in tumor suppressor genes and proto-oncogenes. Specific DNA mutations in a parathyroid cell may confer a proliferative advantage over normal neighboring cells, thus allowing for clonal growth.:
- Large populations of these altered cells containing the same mutation within hyper functioning parathyroid tissue suggest that such glands are a result of clonal expansion
- The majority of PHPT cases are sporadic
- Nonetheless, PHPT also occurs within the spectrum of a number of inherited disorders such as:
- Multiple endocrine neoplasia syndromes (MEN):
- MEN type 1 (Wermer Syndrome
- MEN type 2A (Sipple Syndrome)
- Isolated familial HPT
- Familial HPT with jaw-tumor syndrome
- Multiple endocrine neoplasia syndromes (MEN):
- All of these syndromes are inherited in an:
- Autosomal dominant fashion
- Although exposure to low-dose therapeutic ionizing radiation and familial predisposition account for some cases:
#Arrangoiz #ParathyroidSurgeon #ParathyroidExpert #Hyperparathyroidism #PrimaryHyperparathyroidism #CancerSurgeon #EndocrineSurgery #Teacher #Surgeon #HeadandNeckSurgeon #SurgicalOncologist #ParathyroidAdenoma #Hypercalcemia #ElevatedCalciumLevels #Miami #MountSinaiMedicalCenter #MSMC #Mexico #Hialeah