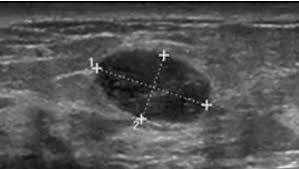
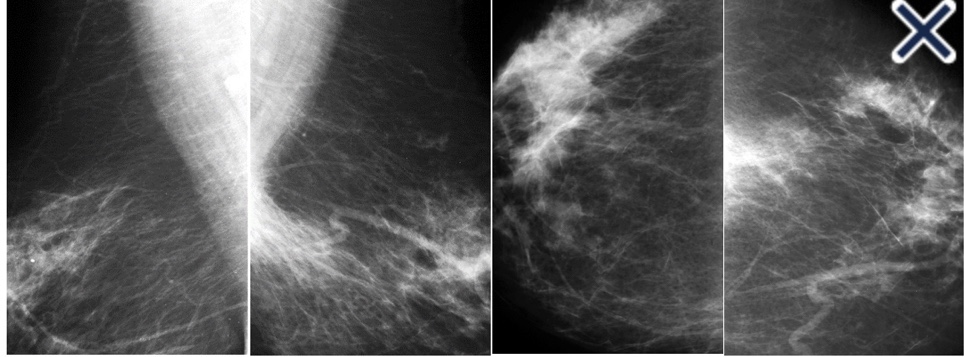
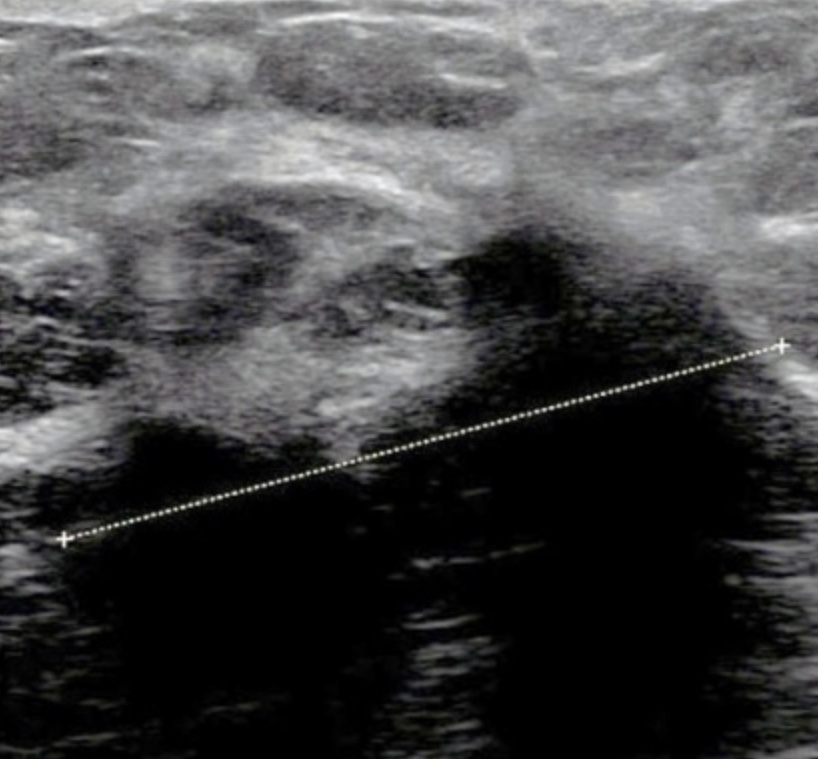
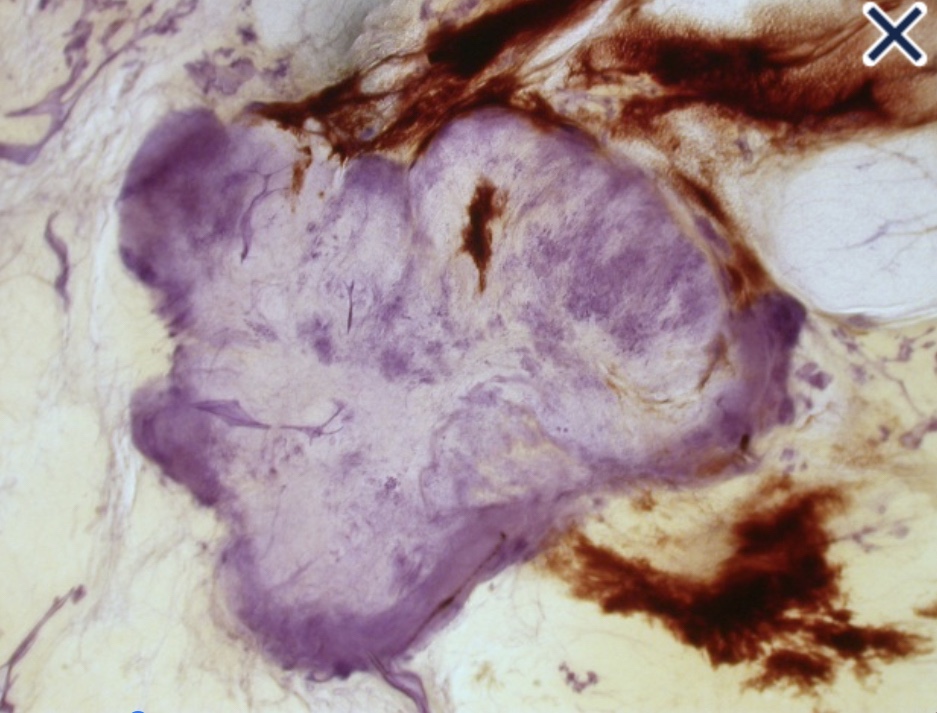
- In women with hormone receptor positive (HR+), HER2-negative early breast cancer, the 21-gene signature score:
- Provides prognostic information that is independent of clinicopathological features
- A high score (on a scale of 0 to 100) indicates:
- A higher rate of distant recurrence and is predictive of chemotherapy benefit
- The prospective Trial Assigning Individualized Options for Treatment (TAILORx);
- Showed that endocrine therapy alone was noninferior to adjuvant chemotherapy plus endocrine (chemoendocrine) therapy:
- In women with HR+, HER2-negative, axillary node-negative breast cancer and a 21-gene recurrence score of 11 to 25
- An exploratory analysis indicated some benefit of chemotherapy:
- In women 50 years of age or younger who had a recurrence score of 16 to 25
- In this analysis there was a small (~1.6%) chemotherapy benefit in distant disease-free survival for patients with recurrence score results from 16 to 20, and a modest (~6.5%) chemotherapy benefit for patients with recurrence score results from 21 to 25
- Showed that endocrine therapy alone was noninferior to adjuvant chemotherapy plus endocrine (chemoendocrine) therapy:
References
1. Sparano JA, Gray RJ, Ravdin PM, Makower DF, Pritchard KI, Albain KS, et al. Clinical and genomic risk to guide the use of adjuvant therapy for breast cancer. New Engl J Med. 2019;380(25):2395-2405.
2. Sparano JA, Gray RJ, Makower DF, Pritchard KI, Albain KS, Hayes DF, et al. Adjuvant chemotherapy guided by a 21-gene expression assay in breast cancer. New Engl J Med. 2018;379(2):111-121.