RET / PTC rearrangement is another genetic alteration that is frequently found in papillary thyroid carcinomas (PTC), and is a result of the fusion between the 3´-portion of the RET receptor tyrosine kinase gene and the 5´-portion of various genes.
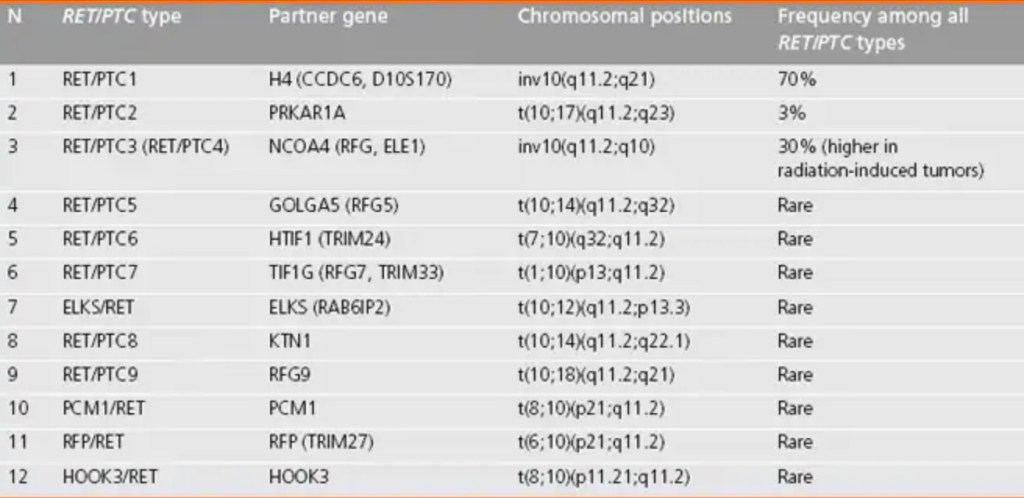
Two most common rearrangement types, RET / PTC1 and RET / PTC3, are paracentric inversions, because both RET and its respective fusion partner, H4 or NCOA4 (ELE1), reside on the long arm of chromosome 10.
RET / PTC2 and nine more recently identified types of RET / PTC are all interchromosomal translocations. Most of these rare RET / PTC types have been found in papillary thyroid carcinomas from patients with a history of either environmental or therapeutic exposure to ionizing radiation, with the exception of the ELKS-RET and HOOK3-RET fusions, which have been identified in papillary thyroid carcinoma with no apparent history of radiation exposure.
All fusions leave the tyrosine kinase domain of the RET receptor intact and enable the RET / PTC oncoprotein to bind SHC and activate the RAS-RAF-MAPK cascade.
RET / PTC is found on average in approximately 20% of adult sporadic papillary thyroid carcinomas, although its prevalence is highly variable between different observations due to either geographic variability or different sensitivity of the detection.
RET / PTC fusion is typically more common in tumors from patients with a history of radiation exposure (50% to 80%) and in papillary thyroid carcinomas from children and young adults (40% to 70%).
The distribution of RET / PTC rearrangement within the tumor may be quite heterogeneous and vary from involving almost all neoplastic cells (clonal RET / PTC) to being detected only in a small fraction of tumor cells (nonclonal RET / PTC).
Although RET / PTC has been found in several studies in adenomas and other benign thyroid lesions, it can be assumed that clonal RET / PTC (i.e., rearrangement that is found in most cells within the tumor) is reasonably specific for papillary thyroid carcinomas.
RET / PTC rearrangements can be detected in thyroid FNA samples. Several studied have shown that RET / PTC detection can refine the preoperative diagnosis of thyroid nodules, particularly in samples that are indeterminate by cytology or have insufficient amount of cells for cytological evaluation. Although these studies have provided important evidence for potential diagnostic utility in RET / PTC detection in thyroid FNA samples, the performance characteristics of this test must be defined in a large prospective study before considering the implementation of this test into clinical practice. One potential problem with such a test lies in the requirement for isolation of acceptable quality RNA, which is difficult to achieve in the fixed samples. This limitation can be resolved by collecting a small portion of the aspirated FNA material directly into nucleic acid preservative solution. This approach typically yields sufficient quality and quantity of RNA that can be used for successful RET / PTC testing.
Papillary thyroid carcinomas with RET / PTC rearrangements typically present at a younger age and have a high rate of lymph node metastases, classic papillary histology and lower stage at presentation, particularly those harboring RET / PTC1
In papillary thyroid carcinomas associated with exposure to ionizing radiation (i.e., post-Chernobyl tumors), RET / PTC1 was found to be associated with classic papillary histology, whereas RET / PTC3 type was more common in the solid variant.

called H4 (B).

