
- Several drugs have been reported to cause a drug-induced thyroiditis:
- Amiodarone
- Interferon-alfa
- Interleukin-2
- Lithium:
- Lithium has been reported to cause a non destructive thyroiditis:
- Similar to sporadic silent thyroiditis.
- Lithium has been reported to cause a non destructive thyroiditis:
- Minocycline
- The clinical course of the drug induced thyroiditis is similar to the other forms of destructive thyroiditis:
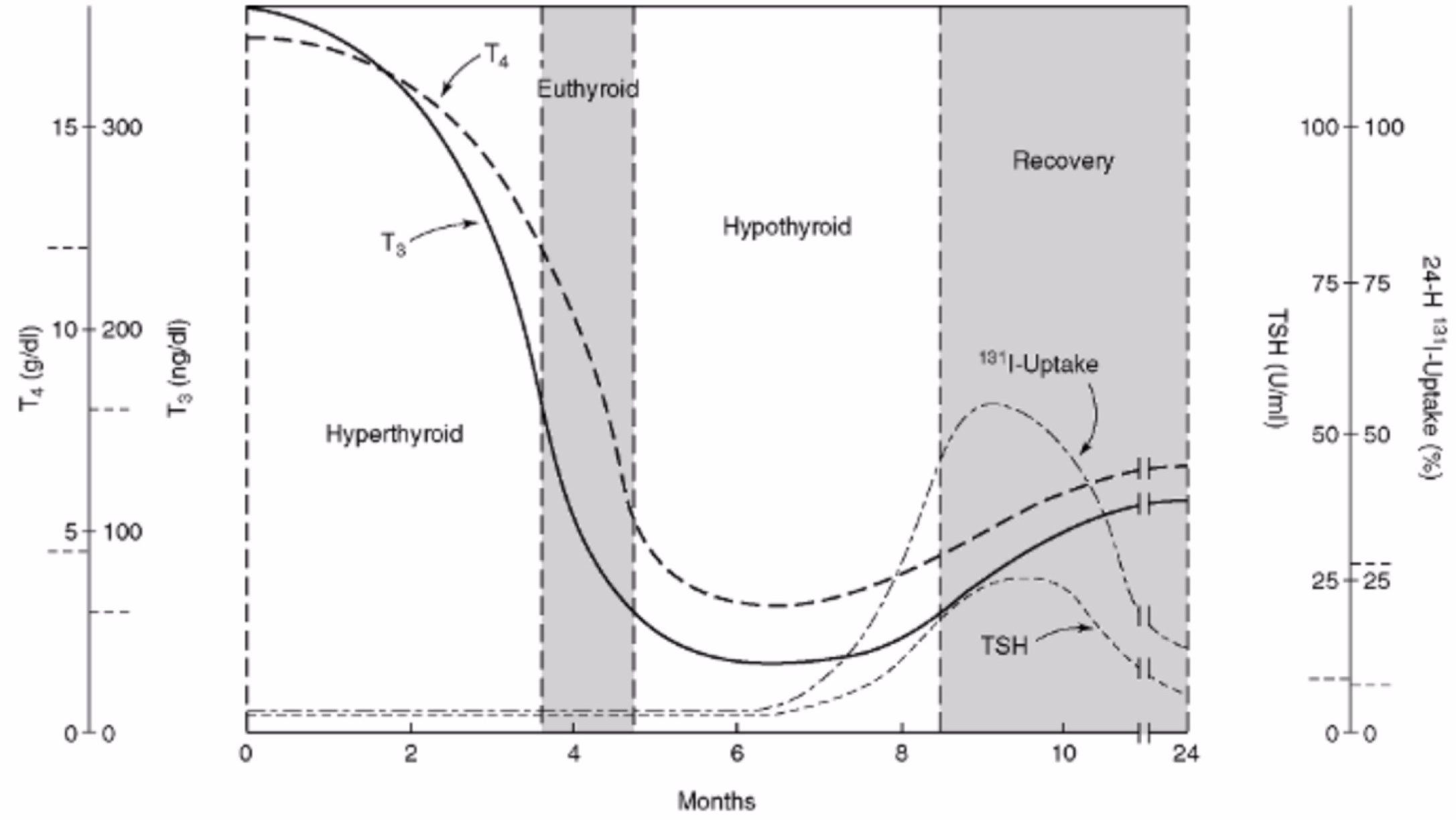
- Importantly:
- Patients on the offending drugs may also develop:
- Subacute, sporadic, or suppurative thyroiditis:
- So these diagnoses need to be evaluated before ascribing the thyroiditis to a drug.
- Subacute, sporadic, or suppurative thyroiditis:
- Patients on the offending drugs may also develop:
- The thyroid abnormalities usually resolve with discontinuation of the offending drug.
- Two drugs that deserve special mention are amiodarone and interferon-alfa:
- Amiodarone:
- An iodine-rich drug used in the treatment of cardiac arrhythmias:
- Is well recognized to produce thyrotoxicosis by two forms:
- Iodine-induced hyperthyroidism (type I)
- Destructive thyroiditis (type II)
- Is well recognized to produce thyrotoxicosis by two forms:
- Distinguishing between the two forms is often a diagnostic dilemma:
- And occasionally both forms may be present in the same patient.
- In general:
- Type II amiodarone-induced thyrotoxicosis occurs in:
- A previously normal thyroid
- The 24 RAIU is completely suppressed
- Color flow Doppler ultrasonography shows absent vascularity.
- Type II amiodarone-induced thyrotoxicosis occurs in:
- The thyrotoxicosis usually responds to:
- High doses of prednisone (40 to 60 mg daily):
- Consistent with the underlying inflammatory process.
- In all cases of amiodarone-induced thyrotoxicosis:
- The drug should be discontinued if at all possible.
- High doses of prednisone (40 to 60 mg daily):
- An iodine-rich drug used in the treatment of cardiac arrhythmias:
- Interferon-alpha:
- Is an immunomodulatory drug that is used in a variety of clinical conditions:
- Most commonly in the treatment of viral hepatitis.
- Up to 70% of patients without previous thyroid autoimmunity will develop:
- High serum thyroid peroxidase antibody concentrations during interferon therapy.
- Like amiodarone; two forms of interferon-induced thyrotoxicosis have been described:
- A Graves’-like hyperthyroidism
- A destructive thyroiditis
- Frequently:
- The thyrotoxicosis is mild and symptomatic therapy is often all that is necessary.
- Because treatment with interferon-alpha is for a defined period:
- The drug usually can be continued to finish the course of therapy when thyroid dysfunction develops.
- Thyroid function usually normalizes after the interferon is stopped:
- However, affected patients are at increased risk for autoimmune thyroid dysfunction in the future
- Is an immunomodulatory drug that is used in a variety of clinical conditions:
- Amiodarone:
#Arrangoiz #CancerSurgeon #ThyroidSurgeon #ParathyroidSurgeon #HeadandNeckSurgeon #ThyroidExpert #SurgicalOncologist #EndocrineSurgery #MountSinaiMedicalCenter #Miami #ThyroidNodule #ToxicNodularGoiter #TNG #MultinodularGoiter #GravesDisease #Hyperthyroidism #Goiter #DrugInducedThyroiditis
