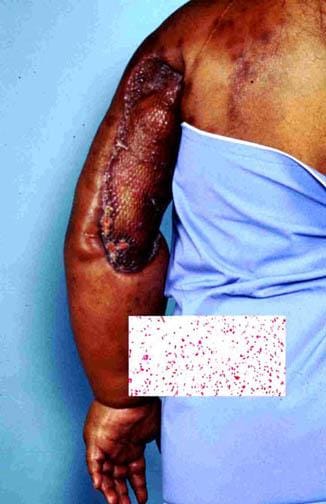
- Stewart-Treves syndrome:
- Is a rare complication of longstanding lymphedema
- It is a deadly cutaneous angiosarcoma
- Most commonly, this tumor is a result of lymphedema induced by radical mastectomy to treat breast cancer:
- Unfortunately, although the breast cancer may be cured with such radical surgery:
- This second primary cancer may be responsible for the patient’s worsening course.
- Unfortunately, although the breast cancer may be cured with such radical surgery:
- The term Stewart-Treves syndrome is broadly applied to an angiosarcoma that arises in a chronically lymphedematous region due to any cause, including:
- Congenital lymphedema and other causes of secondary lymphedema unassociated with mastectomy
- As reported by Durr et al in 2004, this lymphangiosarcoma occurs as a rare complication:
- Lymphangiosarcoma is a misnomer because this malignancy seems to arise from blood vessels instead of lymphatic vessels:
- A more appropriate name is hemangiosarcoma
- Lymphangiosarcoma is a misnomer because this malignancy seems to arise from blood vessels instead of lymphatic vessels:
- In 1906, Lowenstein first described angiosarcoma:
- In a patient’s arm that had been affected by severe posttraumatic lymphedema for 5 years
- In 1948, Stewart and Treves reported this rare secondary malignancy in six cases of angiosarcoma in postmastectomy lymphedema:
- They recognized that an edematous arm after radical mastectomy for breast cancer may suggest recurrent breast cancer:
- But that long-standing chronic edema without recurrent cancer may occasionally produce “a heretofore unrecognized and unreported sequel … long after the malignant breast neoplasm has apparently been arrested … a new specific tumor”
- Stewart and Treves suggested that these angiosarcomas were probably not observed previously because they were mistaken for recurrent, inoperable, cutaneous manifestations of breast cancer
- They recognized that an edematous arm after radical mastectomy for breast cancer may suggest recurrent breast cancer:
- Clinical suspicion should be high:
- As this syndrome is easily misdiagnosed and treatment is advertently delayed
- Pathophysiology:
- The pathogenic mechanism by which lymphedema may induce angiosarcoma has been the subject of controversy
- Stewart and Treves found a high incidence of third malignancies in patients with postmastectomy angiosarcoma:
- Thus, they speculated that a systemic carcinogenic factor was the main causative factor in the pathogenesis of lymphangiosarcomas.
- In 1979, Schreiber and others postulated the concept of local immunodeficiency in the presence of lymphedema:
- This theory is supported by experimental evidence:
- In 1960, Stark and associates demonstrated that homograft skin transplanted to lymphedematous arms survive much longer than those transplanted to healthy arms:
- Therefore, lymphedema may cause some degree of local immunodeficiency and lead to oncogenesis
- In 1960, Stark and associates demonstrated that homograft skin transplanted to lymphedematous arms survive much longer than those transplanted to healthy arms:
- This theory is supported by experimental evidence:
- The possibility that radiation therapy has an important role in the induction of lymphangiosarcoma is also postulated:
- Sternby et al reported that in their study:
- The patient with the shortest interval between radical mastectomy and the onset of the tumor (8 months) received both preoperative radiation therapy of the breast and involved axillary lymph nodes followed by fractionated radiation
- Others suggest that irradiation is not an essential factor in the pathogenesis of this tumor
- Finally, irradiation may be an indirect cause of lymphangiosarcomas because it may cause axillary node sclerosis and thereby accelerate and aggravate the edema
- Sternby et al reported that in their study:
- Clinical data from Swedish women with previous breast cancer who developed angiosarcomas / lymphangiosarcomas on the thoracic wall / upper extremity between 1958 and 2008:
- Showed 31 angiosarcomas developed at a median age of 71 years
- The 14 women treated for breast cancer with radical mastectomy and radiotherapy from 1949 to 1988 developed angiosarcomas in edematous arms after a median 11 years
- Whereas 17 females treated by segmental resection, antihormonal treatment, and radiotherapy from 1980 to 2005 developed angiosarcomas in the irradiated field on the thoracic wall after a median 7.3 years
- Epidemiology:
- Frequency:
- Currently, approximately 400 cases of Stewart-Treves syndrome are reported in the world literature
- In 1962, Schirger calculated that the incidence of this disease is 0.45% in patients who survive at least 5 years after radical mastectomy
- Another analysis calculated it as occurring in 0.03% of patients surviving 10 or more years after radical mastectomy:
- As a result of the increase in conservative treatment for breast carcinoma and improvement of operative and radiation therapy techniques:
- The prevalence of Stewart-Treves syndrome has decreased
- As a result of the increase in conservative treatment for breast carcinoma and improvement of operative and radiation therapy techniques:
- Race:
- No racial predominance exists for Stewart-Treves syndrome
- Gender:
- Most patients with Stewart-Treves syndrome are women with a history of breast cancer that has been treated with radical mastectomy:
- Which causes chronic lymphedema
- Most patients with Stewart-Treves syndrome are women with a history of breast cancer that has been treated with radical mastectomy:
- Age:
- Stewart-Treves syndrome usually occurs in middle-aged or elderly women, a few years or many years after mastectomy:
- In 1981, Sordillo and associates reported a peak incidence in persons aged 65 to 70 years
- In 1972, Woodward et al described a series of 23 patients in a review of 163 cases of Stewart-Treves syndrome from the literature:
- They recorded an average patient age of 68.8 years at the onset of lymphangiosarcoma:
- The youngest patient was aged 44 years and the oldest, 84 years
- They recorded an average patient age of 68.8 years at the onset of lymphangiosarcoma:
- Frequency:
- Once diagnosed:
- Surgical excision is the treatment of choice, sometimes requiring forequarter amputation
- Early amputation or wide local excision provides the best chance of long-term survival in patients with Stewart-Treves syndrome
- Some authorities favor radical ablative surgery with an early diagnosis, in order to confer a reasonable prognosis with this rare but aggressive disease
- A nihilistic approach is undesirable
- The most common approach in patients with lymphangiosarcoma is amputation of the limb or forequarter rather than wide local surgical excision
- Even in cases with early surgical treatment, the prognosis is disappointing, with a high rate of local recurrence and metastasis
- Metastatic disease should exclude surgical treatment unless surgery is useful for symptomatic improvement
- Chemotherapy may have some role:
- However its benefit is unclear
- Chemotherapy and irradiation continue to be evaluated as adjuvants to surgery for the treatment of Stewart-Treves syndrome:
- Currently, these treatment options offer little benefit
- Multiple studies have shown the 5-year survival to be very poor:
- At less than 10%
- The mean survival is 20 months
- Multimodal therapy including:
- Hyperthermic isolated limb perfusion with tumor necrosis factor-alpha and melphalan, combined with radical resection of the affected skin and subcutaneous tissue including the fascia, with large safety margins, may provide enhanced survival
- In 2000, Grobmyer and associates found no statistical significant difference in the survival rates of patients treated with chemotherapy compared with those treated with irradiation:
- Although long-term survivors after either radiation therapy or systemic chemotherapy have been reported:
- The overall results have been discouraging
- Although long-term survivors after either radiation therapy or systemic chemotherapy have been reported:
- A questionable response to weekly paclitaxel has been described:
- As a result of these findings, these treatment options are reserved for patients with inoperable, advanced disease or those who refuse surgery
- Intra-arterial mitoxantrone / paclitaxel was used for angiosarcoma of the lower limb associated with chronic lymphedema (Stewart-Treves syndrome) in a patient with cervical cancer
- In 1994, Furue et al demonstrated that immunotherapy may be beneficial as palliative treatment for pleural effusions caused by metastatic angiosarcoma:
- Expression of VEGF-C makes this angiosarcoma a good potential candidate for targeted antilymphangiogenic therapy
- Stewart-Treves syndrome occurring in the abdominal wall was successfully treated with eribulin mesylate:
- A structurally modified analog of halichondrin B, originally isolated from the marine sponge Halichondria okadai
- References
- Cui L, Zhang J, Zhang X, et al. Angiosarcoma (Stewart-Treves syndrome) in postmastectomy patients: report of 10 cases and review of literature. Int J Clin Exp Pathol. 2015;8(9):11108-11115.
- Penel N, Bui BN, Bay JO, et al. Phase II trial of weekly paclitaxel for unresectable angiosarcoma: the ANGIOTAX Study. J Clin Oncol. 2008;26(32):5269-5274.
- Stewart FW, Treves N. Lymphangiosarcoma in postmastectomy lymphedema: A report of six cases in elephantiasis chirurgica. Cancer. 1948. 1:64-81.
- Hallel-Halevy D, Yerushalmi J, Grunwald MH, Avinoach I, Halevy S. Stewart-Treves syndrome in a patient with elephantiasis. J Am Acad Dermatol. 1999 Aug. 41(2 Pt 2):349-50.
- Offori TW, Platt CC, Stephens M, Hopkinson GB. Angiosarcoma in congenital hereditary lymphoedema (Milroy’s disease)–diagnostic beacons and a review of the literature. Clin Exp Dermatol. 1993 Mar. 18(2):174-7.
- Farhat MM, Le Guern A, Peugniez C, Dabouz F, Quinchon JF, Modiano P. [Angiosarcoma in primary lymphoedema: A rare complication]. Ann Dermatol Venereol. 2018 Apr. 145 (4):266-269.
- Schreiber H, Barry FM, Russell WC, Macon WL 4th, Ponsky JL, Pories WJ. Stewart-Treves syndrome. A lethal complication of postmastectomy lymphedema and regional immune deficiency. Arch Surg. 1979 Jan. 114(1):82-5.
- Stark RB, Dwyer EM, De Forest M. Effect of surgical ablation of regional lymph nodes on survival of homografts. Ann NY Acad Sci. 1960. 87:140-148.
- Cabral ANF, Rocha RH, Amaral ACVD, Medeiros KB, Nogueira PSE, Diniz LM. Cutaneous angiosarcoma: report of three different and typical cases admitted in a unique dermatology clinic. An Bras Dermatol. 2017 Mar-Apr. 92 (2):235-238.
- Sternby NH, Gynning I, Hogeman KE. Postmastectomy angiosarcoma. Acta Chir Scand. 1961. 121:420-432.
- Styring E, Fernebro J, Jonsson PE, et al. Changing clinical presentation of angiosarcomas after breast cancer: from late tumors in edematous arms to earlier tumors on the thoracic wall. Breast Cancer Res Treat. 2010 Jan 20.
- Stanczyk M, Gewartowska M, Swierkowski M, Grala B, Maruszynski M. Stewart-Treves syndrome angiosarcoma expresses phenotypes of both blood and lymphatic capillaries. Chin Med J (Engl). 2013 Jan. 126(2):231-7.
- Schirger A. Postoperative lymphedema: etiologic and diagnostic factors. Med Clin North Am. 1962 Jul. 46:1045-50.
- Wierzbicka-Hainaut E, Guillet G. [Stewart-Treves syndrome (angiosarcoma on lyphoedema): A rare complication of lymphoedema]. Presse Med. 2010 Dec. 39(12):1305-8.
#Arrangoiz #BreastSurgeon #CancerSurgeon #SurgicalOncologist #BreastCancer #Angiosarcoma #StewartTrevesSyndrome #CASO #Miami #CenterforAdvancedSurgicalOncologist
