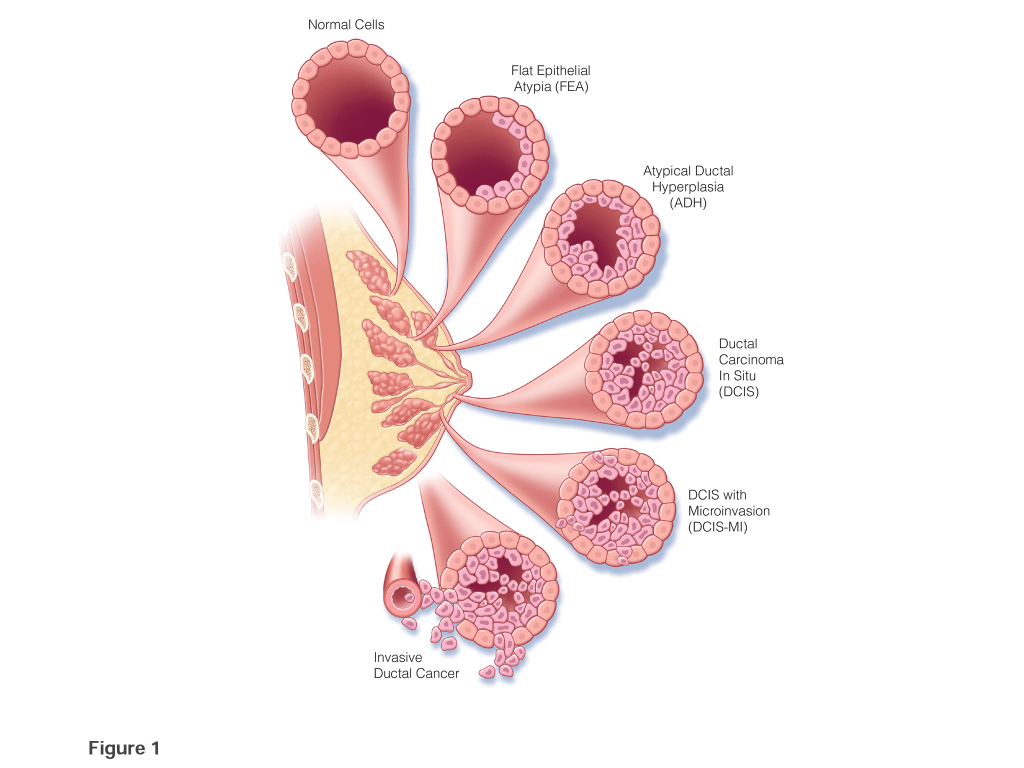
Ductal carcinoma in situ (DCIS) is a malignant intra-ductal proliferation of epithelial cells within the tubular-lobular system of the breast with no microscopic evidence of permeation across the basement membrane. There appears to be a progression between flat epithelial atypia, atypical ductal hyperplasia (ADH), and DCIS, in which DCIS is final step prior to the development of invasive disease. The clinical risk factors and molecular alterations related with malignant transformation are very similar between DCIS and invasive cancer. The concurrence of DCIS and invasive carcinoma within one lesion suggests that DCIS is a precursor lesion to invasive carcinoma. Evidence of the ability of DCIS to progress is that 50% of all recurrences after breast-conserving surgery (BCS) for DCIS, with or without adjuvant treatment, are invasive.
Data is sparse on the natural history of DCIS, but some series have reported the outcomes for women many years after undergoing a surgical biopsy that was interpreted as benign that contained an unrecognized area of DCIS (1–4). These data identified that approximately 20% to 53% of these women developed ipsilateral invasive carcinoma. Sanders et al. reported on 28 women with unrecognized low-grade DCIS in the surgical biopsy specimen, of which 11 developed invasive carcinoma, all of these cancers developed in the same breast and quadrant as the biopsy containing the DCIS (1). The vast majority of these invasive cancers developed within 10 years, but three were diagnosed after 20 years.
Collins et al, in the Nurses’ Health Study, singled out 13 women who were found to have DCIS on reexamination of the surgical biopsies that were previously diagnosed as benign (2). Ten of these women subsequently developed breast cancer; all were ipsilateral, four were DCIS and six were invasive (2). The interval between the biopsy and the progression to invasive cancer was on average nine years.
Approximately one in eight women (i.e., 12%) in the United States (US) will be diagnosed with breast cancer in her lifetime, and 20% to 25% of these newly diagnosed cases will be DCIS (Siegel 2015, CA Cancer J Clin). In 2020, an estimated 48,530 cases of DCIS will be diagnosed in US (American Cancer Society: Cancer Facts and Figures 2020. Atlanta, Ga: American Cancer Society, 2020. Available onlineExit Disclaimer. Last accessed January 17, 2020).
Universal screening mammography has resulted in a 10-fold increase in the incidence of DCIS since the mid-1980s, but since 2003, the incidence of DCIS has decreased in women age 50 years and older, conceivably secondary to decline in the use of hormone replacement therapy, while the incidence in women under 50 continues to increase (Altekruse SF, Kosary CL, Krapcho M, et al.: SEER Cancer Statistics Review, 1975-2007. Bethesda, Md: National Cancer Institute, 2010. Also available online. Last accessed April 3, 2020). Roughly one in every 1,300 mammograms performed in US will lead to a diagnosis of DCIS, representing 17% to 34% of all mammographically detected breast cancers. Before the institution of widespread screening mammography in the mid-1980s, most of the cases of DCIS were not identified until a palpable tumor developed, but today, 80% to 85% of DCIS cases are screen detected.
The incidence of DCIS in necropsy studies is higher than in the general population, proposing that not all DCIS lesions become clinically significant and supporting concerns that most of the increase in DCIS incidence is due to the detection of non-aggressive subtypes that are unlikely to progress to invasive cancer.
Most women with DCIS are diagnosed at a median age that ranges from 47 to 63 years, similar to that reported for patients with invasive carcinoma. However, the age of peak incidence for DCIS (96.7 per 100,000 women), occurs between the ages of 65 and 69 years, which is younger than that for invasive breast cancer, for which peak incidence (453.1 per 100,000 women), occurs between the ages of 75 and 79 years.
The incidence of first-degree relative having breast cancer (i.e., 10% to 35%) as well as rates of deleterious mutations in the breast cancer associated (BRCA) genes are similar for patients with DCIS as for women with invasive breast cancer. Other risk factors for DCIS include: older age, proliferative breast disease, increased breast density, nulliparity, older age at primiparity, history of breast biopsy, early menarche, late menopause, long-term use of postmenopausal hormone replacement therapy, and elevated body mass index in postmenopausal women, are the same as those for invasive breast cancer, but in many cases, the relationship between a given characteristic and invasive cancer is stronger than the relationship between that characteristic and DCIS.
#Arrangoiz #BreastSurgeon #CancerSurgeon #SurgicalOncologist #BreastCancer
