👉BRCA1-associated breast cancer is frequently high-grade basal-type breast cancer.
👉One recent meta-analysis found that BRCA1 mutation was associated with worse survival, but a second recent meta-analysis failed to confirm this.
👉It is becoming apparent that BRCA1/BRCA2-associated breast cancer is more sensitive to chemotherapy of all types than sporadic breast cancer.
👉The outcome for BRCA1/BRCA2-associated breast cancer is likely no worse than that for sporadic breast cancer in the era of multimodal treatment.
👉Breast conservation is an option for nearly any mutation carrier provided that they are willing to accept the risk of second primary breast cancer.
👉The risk of ipsilateral breast tumor events ranges from 1.7% to 2.7% per year, but could be as high as 4% per year for very early onset breast cancer (e.g., age 42 or younger).
👉This risk is modified downward by hormonal therapy for estrogen receptor–positive breast cancer and by chemotherapy.
👉Breast conservation should be avoided in homozygous ATM mutation carriers (i.e., patients with ataxia-telangiectasia) in whom radiation is contraindicated and possibly TP53 mutation carriers, who may be at increased risk for radiation-induced malignancies.
👉Lifetime contralateral breast cancer risk is as high as 62% to 83% for BRCA1/BRCA2 mutation carriers.
👉There is some evidence that bilateral mastectomy improves survival in this population.
👉Although follow-up is limited, available data show acceptable local recurrence risk for BRCA 1 / 2 mutation–associated breast cancer treated by nipple-sparing mastectomy.
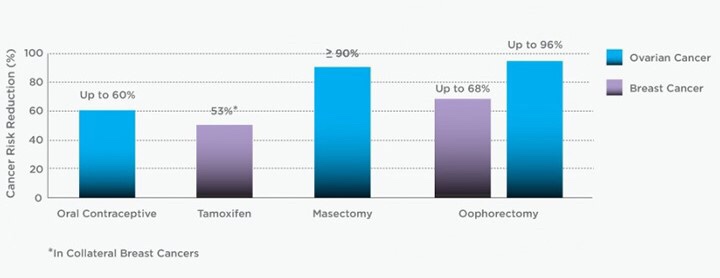
👉It is reasonable to encourage oophorectomy in BRCA1 and BRCA2 mutation carriers who are treated for breast cancer as this may reduce mortality by 43% to 70%, an effect that seems greatest for estrogen receptor–negative breast cancer.
👉Bilateral salpingo-oophorectomy was associated with improved all-cause and breast cancer–specific mortality in BRCA1 mutation carriers with stage 1 to 3 breast cancer.
👉There is evidence that outcome for BRCA 1 / BRCA 2 mutation–associated ovarian cancer is better than for sporadic ovarian cancer.
👉This is particularly true for BRCA2-associated ovarian cancer, which shows enhanced sensitivity to chemotherapy.
👉Nevertheless, ovarian cancer is the main mortality driver for BRCA 1 / BRCA 2 mutation carriers, and clinicians will sometimes be called upon to manage breast cancer risk in patients who have completed ovarian cancer treatment.
👉One recent study that included 364 patients with BRCA 1 / BRCA 2-associated ovarian cancer reported a 10-year survival of 11%, with 10% of patients developing breast cancer.
👉There is growing evidence that BRCA 1 / BRCA 2-associated breast cancer is less sensitive to taxanes than sporadic breast cancer and more sensitive to DNA-damaging agents, such as mitomycin C and platins.
👉BRCA 1 / BRCA 2 mutations also predict sensitivity to poly (ADP-ribose) polymerase (PARP) inhibition.
👉Trials of platin agents and PARP inhibitors consistently identify BRCA 1 / BRCA 2 mutation as the strongest predictor of response.
👉There is a growing list of platinum and PARP inhibitor trials open and accruing for BRCA1 and BRCA2 mutation carriers.
👉Whether this approach will be equally efficacious for individuals with mutations in other DNA repair genes, such as PALB2, RAD51C, BRIP, ATM, and CHEK2, is not certain, but it is hoped that the development and validation of predictive homologous recombination assays will make it possible to prospectively identify the right patients for these agents.
#Arrangoiz #BreastSurgeon #CancerSurgeon #SurgicalOncologist #BreastCancer #HereditaryBreastCancer
