Bilateral Prophylactic Mastectomy
👉A recent meta-analysis that included 2,635 BRCA1/BRCA2 mutation carriers reported a 93% reduction in breast cancer incidence for the 627 women who underwent bilateral risk-reducing mastectomy.
👉Based on the four studies included in this meta-analysis, it can be estimated that baseline breast cancer risk was 1.7% to 2.8% per year for BRCA1/BRCA2 gene mutation carriers (34% to 56% after 20 years) and 0% to 0.8% per year after bilateral risk-reducing mastectomy (0% to 16% after 20 years).
👉Median follow-up was only 3 to 6 years for these studies, so the durability of these estimates is not certain.
👉After mastectomy, terminal duct-lobular units (TDLUs) can be identified in peripheral skin, in the inframammary crease, and in the nipple-areola complex.
👉Although removing the nipple-areola complex reduces the number of residual TDLUs, it is not clear that this is required to achieve an acceptably low breast cancer risk.
👉To date, outcomes for bilateral risk-reducing nipple-sparing mastectomy have been reported for over 300 BRCA1/BRCA2 gene mutation carriers.
👉Incidental breast cancers were identified in 3% to 6%, and with a median follow-up of 33 months, subsequent breast cancers have developed in three patients.
👉Modern nipple-sparing mastectomy should not intentionally leave any breast tissue behind.
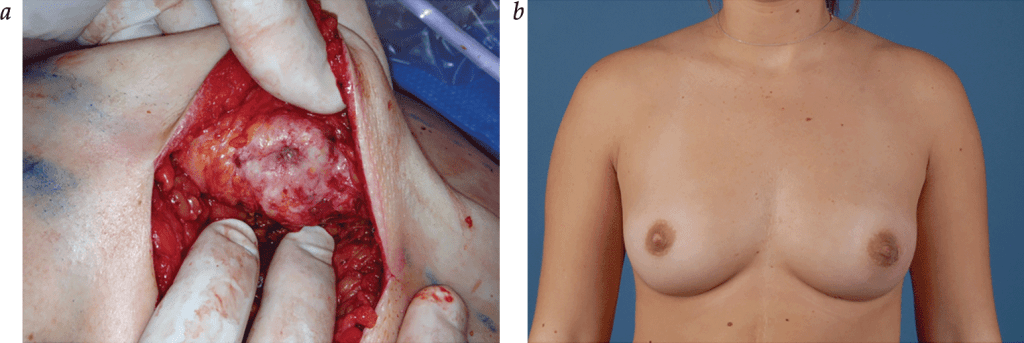
👉Bilateral risk-reducing mastectomy has not yet been shown to improve breast cancer–specific or overall survival in BRCA1/BRCA2 mutation carriers, but a 2010 Cochrane review concluded that risk-reducing mastectomy is likely to confer a survival advantage in the highest-risk women.
#Arrangoiz #BreastSurgeon #BreastCancer #CancerSurgeon #SurgicalOncologist
