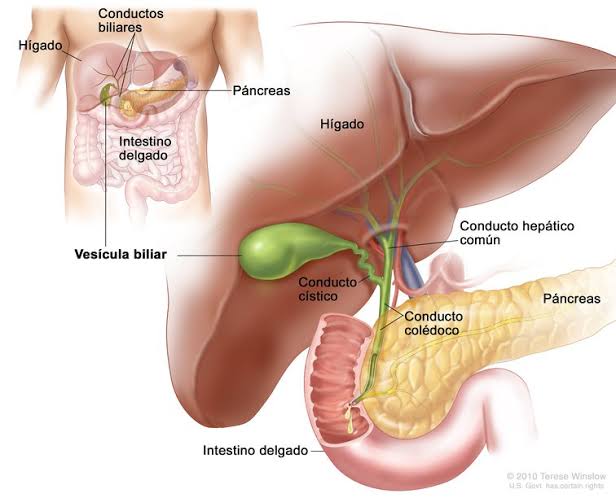
- Introduction:
- Acute pancreatitis:
- Is an acute inflammatory process of the pancreas:
- Mortality ranges from:
- Three percent in patients with interstitial edematous pancreatitis to 17% in patients who develop pancreatic necrosis
- Mortality ranges from:
- Is an acute inflammatory process of the pancreas:
- Acute pancreatitis:
- Classification of Acute Pancreatitis:
- According to the Atlanta classification:
- Acute pancreatitis can be divided into two broad categories:
- Interstitial edematous acute pancreatitis:
- Which is characterized by:
- Acute inflammation of the pancreatic parenchyma and peripancreatic tissues
- But without recognizable tissue necrosis
- Which is characterized by:
- Necrotizing acute pancreatitis:
- Which is characterized by inflammation associated with pancreatic parenchymal necrosis and/or peripancreatic necrosis
- Interstitial edematous acute pancreatitis:
- Acute pancreatitis can be divided into two broad categories:
- According to the severity, acute pancreatitis is divided into the following:
- Mild acute pancreatitis:
- Which is characterized by the absence of organ failure and local or systemic complications
- Moderately severe acute pancreatitis:
- Which is characterized by no organ failure or transient organ failure (less than 48 hours) and/or local complications
- Severe acute pancreatitis:
- Which is characterized by persistent organ failure (greater than 48 hours) that may involve one or multiple organs
- Mild acute pancreatitis:
- According to the Atlanta classification:
- Assessment of Disease Severity:
- At initial evaluation:
- The severity of acute pancreatitis should be assessed by:
- Clinical examination to assess for:
- Early fluid losses
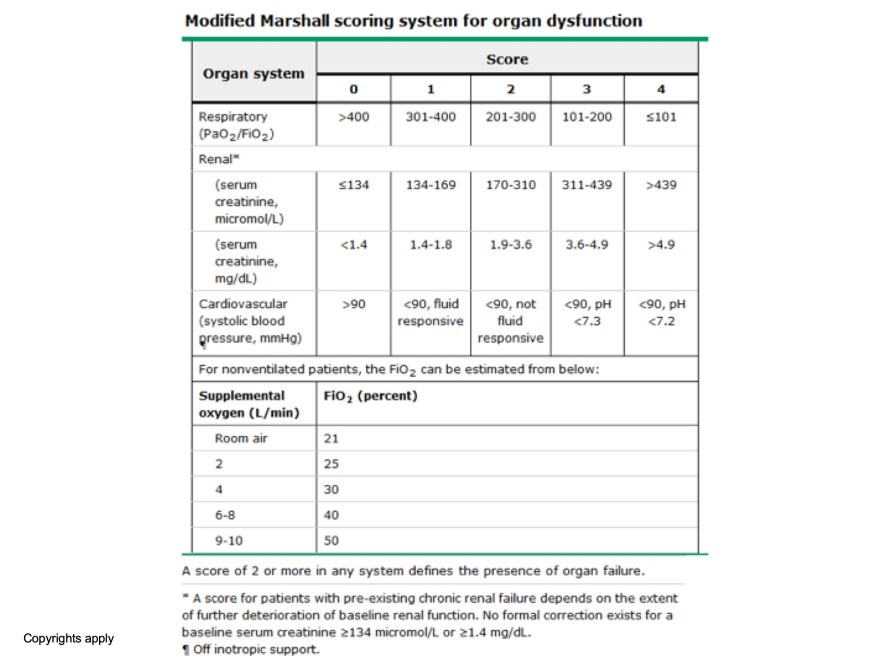
- Organ failure:
- Particularly cardiovascular, respiratory, or renal compromise
- Clinical examination to assess for:
- The severity of acute pancreatitis should be assessed by:
- At initial evaluation:
-
-
-
-
-
- Measurement of the systemic inflammatory response syndrome (SIRS) score
-
-
-
-

-
- I perform the following laboratory tests to help establish the severity of acute pancreatitis and guide management:
- These include a:
- Complete metabolic panel
- Serum calcium
- Complete blood count
- Serum triglycerides
- Lactate
- Although measurement of serum amylase and lipase is useful for diagnosis of pancreatitis:
- Serial measurements in patients with acute pancreatitis are not useful to predict disease severity, prognosis, or for altering management
- These include a:
- Routine abdominal computed tomography (CT) scan:
- Is not recommended at initial presentation in patients with acute pancreatitis unless there is diagnostic uncertainty:
- Because there is no evidence that CT improves clinical outcomes:
- And the complete extent of pancreatic and peripancreatic necrosis may only become clear 72 hours after the onset of acute pancreatitis
- Because there is no evidence that CT improves clinical outcomes:
- Is not recommended at initial presentation in patients with acute pancreatitis unless there is diagnostic uncertainty:
- Several other scoring systems also exist to predict the severity of acute pancreatitis based upon:
- Clinical, laboratory, radiologic risk factors, and serum markers but can be used only 24 to 48 hours after disease onset and have not been shown to be consistently superior to assessment of SIRS or the APACHE II score.
- I perform the following laboratory tests to help establish the severity of acute pancreatitis and guide management:
- Indications for monitored or intensive care:
- Admission to an intensive care unit setting is indicated in the following patients:
- Patients with severe acute pancreatitis
- Patients with acute pancreatitis and one or more of the following parameters:
- Pulse less than 40 or greater than 150 beats/minute
- Systolic arterial pressure less than 80 mmHg or mean arterial pressure less than 60 mmHg or diastolic arterial pressure greater than 120 mmHg
- Respiratory rate greater than 35 breaths/minute
- Serum sodium less than 110 mmol/L or greater than 170 mmol/L
- Serum potassium less than 2.0 mmol/L or greater than 7.0 mmol/L
- PaO2 less than 50 mmHg
- pH less than 7.1 or greater than 7.7
- Serum glucose greater than 800 mg/dL
- Serum calcium greater than 15 mg/dL
- Anuria
- Coma
- Admission to an intensive care unit setting is indicated in the following patients:
- In patients with severe acute pancreatitis:
- Intensive care unit monitoring and support of pulmonary, renal, circulatory, and hepatobiliary function may minimize systemic sequelae:
- Transfer to a monitored or intensive care unit may be considered in the following patients, although it is not uncommon for these patients to be treated on the floor in centers with significant expertise in acute pancreatitis:
- Persistent (greater than 48 hours) SIRS
- Elevated hematocrit (greater than 44%)
- Blood urea nitrogen (BUN) (greater than 20 mg/dL)
- Creatinine (greater than 1.8 mg/dL)
- Age greater than 60 years
- Underlying cardiac or pulmonary disease, obesity
- Transfer to a monitored or intensive care unit may be considered in the following patients, although it is not uncommon for these patients to be treated on the floor in centers with significant expertise in acute pancreatitis:
- Intensive care unit monitoring and support of pulmonary, renal, circulatory, and hepatobiliary function may minimize systemic sequelae:
Rodrigo Arrangoiz MS, MD, FACS cirujano oncology y miembro de Sociedad Quirúrgica S.C en el America British Cowdray Medical Center en la ciudad de Mexico:
-
Es experto en el manejo de patología quirúrgica compleja:

Training:
• General surgery:
• Michigan State University:
• 2004 al 2010
• Surgical Oncology / Head and Neck Surgery / Endocrine Surgery:
• Fox Chase Cancer Center (Filadelfia):
• 2010 al 2012
• Masters in Science (Clinical research for health professionals):
• Drexel University (Filadelfia):
• 2010 al 2012
• Surgical Oncology / Head and Neck Surgery / Endocrine Surgery:
• IFHNOS / Memorial Sloan Kettering Cancer Center:
• 2014 al 2016

#Arrangoiz
#Surgeon
#Cirujano
#SurgicalOncologist
#CirujanoOncologo
#BreastSurgeon
#CirujanodeMama
#CancerSurgeon
#CirujanodeCancer
#Teacher
#Surgeon
#GeneralSurgeon




